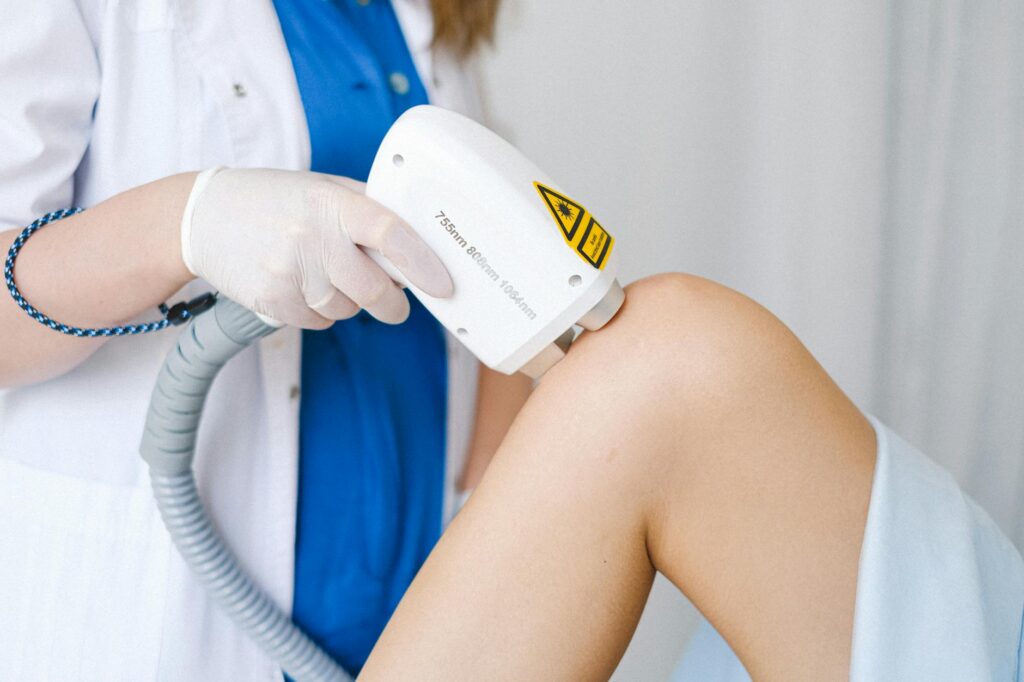
Nd:YAG laser is generally more effective for acne scar pigmentation than Alexandrite, achieving a 38.89% reduction in ECCA (Echelle d’Evaluation Clinique des Cicatrices d’Acné) scores after four monthly treatments, compared to Alexandrite’s 24.7% reduction after three treatments. However, the choice between these two lasers is more nuanced than raw efficacy numbers—it depends on your skin tone, the depth of pigmentation, and whether you’re at risk for post-inflammatory hyperpigmentation (PIH). For someone with lighter skin and superficial post-acne marks, Alexandrite’s 755 nm wavelength offers faster results because it absorbs strongly into melanin sitting near the skin’s surface.
For darker skin types or deeper pigmentation, Nd:YAG’s 1064 nm wavelength is safer because it penetrates without concentrating heat in the melanin layer, reducing the risk of the very problem you’re trying to fix—darkening of the skin. This article breaks down how each laser works, compares their clinical performance, explains skin type considerations, and covers the risk of making pigmentation worse before it gets better. Both lasers represent major advances in treating post-acne hyperpigmentation, but they operate on different principles. Understanding which one suits your specific situation—and your skin—is the key to avoiding wasted time and money.
Table of Contents
- How Do Alexandrite and Nd:YAG Laser Wavelengths Differ in Treating Acne Pigmentation?
- Which Laser Is More Effective for Acne Scar Pigmentation?
- Does Skin Tone Matter When Choosing Between Alexandrite and Nd:YAG?
- What About Post-Inflammatory Hyperpigmentation Risk?
- Picosecond vs Nanosecond: Why Technology Matters for These Lasers
- Can Nd:YAG Fix Alexandrite-Related Side Effects?
- Combining Lasers and Realistic Expectations
- Conclusion
How Do Alexandrite and Nd:YAG Laser Wavelengths Differ in Treating Acne Pigmentation?
The fundamental difference lies in wavelength and how that wavelength interacts with melanin in the skin. Alexandrite operates at 755 nm, a wavelength that is highly absorbed by melanin, making it excellent at targeting the pigmented structures that cause post-acne marks. Nd:YAG lasers come in two variants: 1064 nm (the primary wavelength) and 532 nm (the secondary wavelength). The 1064 nm setting penetrates much deeper into the skin with lower melanin absorption, while the 532 nm setting targets more superficial pigmentation similarly to Alexandrite.
This means that when you’re treating acne pigmentation with each laser, you’re essentially choosing between surface-level precision (Alexandrite or 532 nm) or deeper penetration with gentler melanin interaction (1064 nm). For acne scars and post-inflammatory hyperpigmentation, the choice affects treatment speed and safety. Alexandrite’s strong melanin absorption means it works faster on surface pigment—ideal if you have light to medium skin and want visible improvement within a few sessions. However, that strong melanin absorption is also why it carries higher risk in certain skin types, as we’ll discuss later. Nd:YAG’s lower melanin absorption at 1064 nm makes it safer for darker skin because the laser energy passes through melanin rather than concentrating in it, but this also means it may take slightly longer to achieve results on purely surface-level pigmentation.

Which Laser Is More Effective for Acne Scar Pigmentation?
When it comes to measured clinical outcomes, Nd:YAG pulls ahead in the data. picosecond Nd:YAG reduced ECCA scores—a standardized measure of acne scar severity—by 38.89% after four monthly treatments, whereas picosecond Alexandrite achieved a 24.7% reduction after three treatments. In separate Asian patient populations, picosecond Nd:YAG at 1064 nm achieved even more impressive results: a 54.6% ECCA reduction, outperforming other technologies like erbium-glass fractional lasers. This performance edge makes Nd:YAG the go-to choice when your goal is measurable scar improvement rather than just cosmetic lightening of pigmentation.
The reason for this difference relates to how deeply and comprehensively each laser can address scar tissue. Alexandrite’s strength lies in immediate surface correction—if your post-acne marks are purely pigmentation without significant textural scarring, Alexandrite may feel like the faster choice. But once you add textural scarring into the equation (which most acne damage includes), Nd:YAG’s ability to stimulate deeper collagen remodeling becomes evident. However, if you have only superficial, purely pigmented marks without scar texture, Alexandrite could still deliver noticeable results within fewer sessions. The limitation here is that acne damage is rarely purely pigmented; it usually combines color, texture, and depth, which is where Nd:YAG’s broader capability shines.
Does Skin Tone Matter When Choosing Between Alexandrite and Nd:YAG?
Skin tone is perhaps the most critical factor in choosing between these two lasers, and it’s where Alexandrite’s otherwise attractive efficacy becomes risky. For lighter skin types (Fitzpatrick I-IV), Alexandrite is more effective for rapid results because the light is readily absorbed by surface melanin with less risk of complication. For darker skin (Fitzpatrick IV-VI), Nd:YAG’s 1064 nm wavelength is strongly preferred because its lower melanin absorption means you get therapeutic effect without disproportionately heating the melanin layer itself. The reason this matters is post-inflammatory hyperpigmentation.
Long-pulsed Alexandrite carries a documented high risk of PIH in Asian and darker skin patients, particularly when treating epidermal (surface-level) pigmented lesions. In contrast, Nd:YAG’s gentler interaction with melanin reduces this risk significantly. If you have darker skin and an Alexandrite treatment goes wrong, you may end up with the exact problem you were trying to solve—more pigmentation, not less. This is not rare; it’s a documented clinical concern in the dermatology literature.

What About Post-Inflammatory Hyperpigmentation Risk?
PIH—when the skin responds to laser treatment by becoming darker rather than lighter—is the dark side of laser pigmentation treatment, and it occurs more frequently with Alexandrite, especially in Asian and darker-skinned patients. This isn’t a hypothetical concern; studies document that long-pulsed Alexandrite lasers can trigger PIH when treating surface pigmentation in susceptible populations. The good news: when PIH does occur, it’s often temporary. In a study using 755 nm picosecond Alexandrite, 78.9% of PIH cases resolved within three months, suggesting that the darker pigmentation after treatment was a temporary inflammatory response rather than permanent damage.
However, there’s an important caveat: waiting three months for PIH to resolve is not ideal if you had the laser treatment specifically to improve your appearance. This is where Nd:YAG becomes the practical choice for higher-risk skin types—you’re less likely to trigger PIH in the first place. And if you do develop PIH from any laser treatment, Nd:YAG can treat it: in documented cases, Q-switched Nd:YAG with low fluence successfully improved all Alexandrite-induced PIH lesions after eight sessions, essentially reversing the unwanted darkening. The implication is clear: if you have darker skin, starting with Nd:YAG avoids the PIH problem entirely, whereas using Alexandrite and hoping for resolution puts you in a position where you might need additional treatment to fix the complications.
Picosecond vs Nanosecond: Why Technology Matters for These Lasers
Both Alexandrite and Nd:YAG come in different technology generations, and the difference between picosecond and nanosecond versions meaningfully affects outcomes and side effects. Picosecond lasers deliver energy in trillionths of a second, whereas nanosecond lasers deliver it in billionths of a second. This seemingly tiny difference translates to something crucial: picosecond technology minimizes thermal (heat) damage to surrounding tissue while still targeting and fragmenting melanosomes (the pigment particles). This is why the clinical data showing impressive ECCA reductions and low PIH rates comes predominantly from picosecond systems, not older nanosecond versions.
When you choose a laser treatment, ensure you’re getting picosecond technology if possible, especially if you’re in a higher-risk skin category. Picosecond Nd:YAG achieved that 38.89% ECCA reduction and the 54.6% reduction in Asian patients, and picosecond Alexandrite showed manageable PIH with 78.9% resolution. Older nanosecond systems may work, but the clinical evidence is stronger for picosecond variants, and the side effect profile is better. This is why treatment clinic choice—ensuring they have modern picosecond equipment rather than outdated nanosecond systems—is as important as choosing the wavelength itself.
Can Nd:YAG Fix Alexandrite-Related Side Effects?
One compelling practical finding from dermatology research is that Nd:YAG can actually treat complications from Alexandrite laser when things go wrong. If you’ve had Alexandrite treatment and developed unwanted PIH (the skin darkened instead of lightened), Q-switched Nd:YAG with conservative fluence settings can address it. In clinical documentation, all lesions improved after eight sessions of low-fluence Q-switched Nd:YAG. This cross-treatment capability suggests that if your clinician has access to both technologies, Nd:YAG becomes a safety net—you can attempt Alexandrite on appropriate candidates and pivot to Nd:YAG if adverse pigmentation develops.
However, this shouldn’t be viewed as a reason to choose Alexandrite first and “fix it later” with Nd:YAG. Prevention is always better than correction. Choosing the right laser from the start—especially if you have darker skin—spares you months of additional treatments. The fact that Nd:YAG can reverse Alexandrite-induced PIH is useful information if complications arise, but it underscores why dermatologists now routinely recommend Nd:YAG as the first-line choice for darker skin types.
Combining Lasers and Realistic Expectations
The future of acne pigmentation treatment increasingly involves using both wavelengths strategically in the same patient rather than choosing one or the other. Some advanced clinics use Alexandrite for surface pigmentation in low-risk patients and reserve Nd:YAG for deeper scarring, darker skin, or retreatment. This hybrid approach allows clinicians to leverage each laser’s strengths while minimizing weaknesses. For someone with mixed acne damage—some superficial discoloration and some textural scarring—a combination protocol might deliver superior results to either laser alone.
Set realistic expectations regardless of which laser you choose: a single treatment will not erase acne marks. The data consistently shows that improvement requires multiple sessions (typically three to four for Alexandrite, four or more for Nd:YAG) spaced four weeks apart. Even after a full treatment series, some pigmentation or texture may remain, particularly if the scarring is deep or severe. However, most patients see meaningful improvement—the 24% to 39% ECCA reductions in the clinical studies represent real, visible differences, even if not complete clearance. Patience and realistic goals prevent disappointment.
Conclusion
For most patients seeking to treat acne pigmentation, Nd:YAG laser is the more effective and safer choice, particularly if you have darker skin, mixed scarring, or concerns about post-inflammatory hyperpigmentation. Its 38.89% measured improvement in scar appearance, lower PIH risk, and ability to address both superficial pigmentation and deeper textural damage make it the current gold standard. Alexandrite remains valuable for lighter-skinned patients with purely surface-level pigmentation who want faster results, but the clinical evidence and safety profile favor Nd:YAG as the first-line recommendation across most skin types.
Before committing to treatment, verify that your clinic has modern picosecond technology, not outdated nanosecond systems, and ensure the clinician has experience treating your specific skin type. Ask about their complication rates, expected timeline (usually 4-6 weeks between sessions), and realistic outcome projections for your particular scars. If you have darker skin, specifically request Nd:YAG at 1064 nm and ask about their protocol for minimizing PIH risk. With the right technology, the right provider, and realistic expectations, laser treatment can meaningfully improve post-acne pigmentation and is worth considering if topical treatments have plateaued.
You Might Also Like
- Why Nd:YAG 1064nm Laser Is the Safest for Dark Skin Acne
- What PicoSure Pro Does for Acne Pigmentation and Texture
- What Enlighten III Picosecond Laser Does for Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads