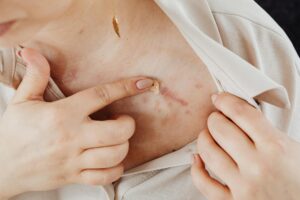
A step-therapy requirement for acne means your insurance company requires you to try and fail lower-cost medications before they’ll approve coverage for the more expensive acne treatment your dermatologist prescribed. Also called “fail-first” protocols, these requirements are cost-control measures that force patients through a prescribed treatment ladder, starting with medications like oral antibiotics or topical retinoids, regardless of whether your dermatologist believes those treatments are appropriate for your specific case. For example, if your doctor prescribes isotretinoin (Accutane) for severe acne, your insurer may deny coverage and require documented proof that you’ve already tried and failed on doxycycline, minocycline, or benzoyl peroxide first—even if your dermatologist determined those treatments wouldn’t work for you. This article explains how step-therapy requirements work, what medications insurers typically require you to try first, how to request exceptions when step therapy isn’t medically appropriate, and what regulatory protections now exist to protect patients from unreasonable delays.
Table of Contents
- How Insurance Step-Therapy Requirements Actually Work for Acne
- Common First-Step Medications Insurers Require Before Expensive Acne Treatments
- Why Insurance Companies Use Step-Therapy Requirements for Acne
- How to Request a Step-Therapy Exception When Your Doctor Disagrees
- Step-Therapy Reform Laws Now Protecting Acne Patients in Some States
- The Real-World Impact of Step-Therapy Delays on Acne Patients
- The Future of Step-Therapy Regulation and Acne Treatment Access
- Conclusion
How Insurance Step-Therapy Requirements Actually Work for Acne
Step-therapy requirements function as a gatekeeping mechanism between you and your prescribed medication. When you go to fill a prescription for an acne treatment, the pharmacy checks your insurance coverage. If the medication is on your plan’s step-therapy list and your insurance records don’t show you’ve completed the required first-step treatments, the pharmacy denies the prescription and contacts your prescriber’s office to request a “step-therapy exception request.” Your doctor then has to submit documentation to your insurance company explaining why the cheaper alternative won’t work for your condition.
The system creates a mandatory waiting period that can last days or weeks while your insurance reviews the exception. Insurance companies argue this process saves money by preventing patients from jumping directly to expensive treatments when cheaper options might work. However, this approach assumes that medications work uniformly across all patients with acne—an assumption dermatologists regularly challenge, since acne severity, type, and treatment response vary dramatically between individuals.

Common First-Step Medications Insurers Require Before Expensive Acne Treatments
Most insurers require patients to try oral antibiotics first. Doxycycline and minocycline are the most common “first steps”—these tetracycline-class antibiotics cost significantly less than newer treatments and have been used for acne for decades. If your insurance denies coverage for a more expensive medication, they typically want documentation that you’ve taken one of these antibiotics for a minimum period, often 4-12 weeks. Topical retinoids like tretinoin or adapalene are also common first-step requirements, and benzoyl peroxide—available over-the-counter—is another treatment insurers expect patients to attempt.
However, if you’ve already tried these medications and they didn’t work for you, that’s exactly when the exception process becomes critical. Some patients are allergic to tetracyclines or experience significant side effects; others have antibiotic-resistant acne that simply doesn’t respond to oral antibiotics. A patient with nodular acne causing permanent scarring has a much stronger case for skipping the step-therapy ladder than a patient with mild comedonal acne. Your dermatologist’s documentation of why the first-step treatment is contraindicated or unlikely to work significantly strengthens your exception request.
Why Insurance Companies Use Step-Therapy Requirements for Acne
Insurance plans use step therapy as a direct cost-containment strategy. A three-month supply of doxycycline might cost $30-50, while isotretinoin for the same period costs $500-3,000 depending on the dosage and whether you’re purchasing brand name Accutane or generic forms. When multiplied across thousands of insured patients, step-therapy requirements create substantial savings for insurers—even if only a small percentage of patients successfully complete the cheaper treatments. The insurance industry frames step therapy as “evidence-based” because these cheaper medications do work for many acne patients, so the logic seems reasonable at a population level.
Yet step therapy creates a fundamental misalignment between insurer incentives and individual patient outcomes. An insurer optimizes for cost across a population; your dermatologist optimizes for the fastest, most effective treatment for your specific case. When your dermatologist has already examined you, assessed your acne severity and type, and determined that you need a specific medication, requiring them to restart with cheaper alternatives wastes time and potentially allows your acne to worsen. A patient with moderate inflammatory acne might benefit from tretinoin alone, but step-therapy requirements force them through antibiotics first, creating a 3-4 month delay for no clinical benefit.

How to Request a Step-Therapy Exception When Your Doctor Disagrees
When your pharmacy denies your prescription due to step-therapy requirements, ask your dermatologist’s office to submit a prior authorization form and step-therapy exception request to your insurance company. This request should include specific medical documentation: your clinical diagnosis, the dermatologist’s assessment of why the required first-step treatment is not appropriate, any previous treatment history showing failed attempts at the required medications, and clinical evidence supporting the prescribed medication. Insurers are required to have a defined timeline for reviewing these requests—typically 24-72 hours for urgent/expedited requests and up to 15 business days for standard requests.
Your insurance company will either approve the exception and authorize your medication, or deny the request and require you to complete the step-therapy protocol. If denied, you have appeal rights; you can request an urgent review if you’re experiencing severe acne or scarring, and your dermatologist can submit additional documentation. Some patients find calling their insurance company directly and asking to speak with a clinical reviewer—rather than relying solely on written requests—accelerates the process. Importantly, if you’ve already tried the required first-step medication in the past (even through a different insurance), mention this in the exception request; insurance companies sometimes waive step-therapy requirements if there’s documented evidence of prior therapeutic failure.
Step-Therapy Reform Laws Now Protecting Acne Patients in Some States
The regulatory landscape for step therapy is changing. New Jersey implemented a significant step-therapy reform law effective January 1, 2026, requiring health plans regulated by the state to establish clear exception and override processes for step-therapy requirements. The law mandates that insurers provide transparency about which medications are subject to step therapy, establish defined timelines for reviewing exception requests (no more than 72 hours for urgent cases), and inform patients of their appeal rights when an exception is denied. This is one of the most comprehensive state-level protections against unreasonable step-therapy delays.
However, protections and requirements vary dramatically by state and insurance plan type. Some states have no specific step-therapy regulations, while others have laws focused on specific conditions (like cancer or specialty medications) but not acne. Additionally, protections differ between types of health plans: state-regulated health insurance plans may have stronger protections than self-insured employer plans, which are governed by federal ERISA law rather than state insurance law. Before filing an exception request, ask your dermatologist’s office which state’s regulations apply to your plan—they often know the specific process your particular insurer uses.

The Real-World Impact of Step-Therapy Delays on Acne Patients
Step-therapy delays create tangible harm, particularly for patients with moderate-to-severe acne who are at risk of permanent scarring. A patient prescribed isotretinoin for nodular acne faces a weeks-long delay while their insurance requires them to complete oral antibiotics first, even though isotretinoin is the only medication proven to clear severe acne permanently. During those weeks, acne lesions continue to form and scar. For many patients, a 4-12 week delay in accessing the medication their dermatologist prescribed represents the difference between skin that clears and skin with permanent scarring that will require future dermatological procedures to address.
Additionally, some patients respond poorly to the required first-step medications, creating an additional delay. A patient might try doxycycline for 8 weeks, experience limited improvement (or side effects like photosensitivity), then file an exception request, wait for approval, and finally start their prescribed medication. A 12-week delay to access the correct treatment translates into months of unnecessary acne progression. This is why dermatologists consider step-therapy requirements particularly problematic for acne—unlike many other conditions where trying cheaper medications first doesn’t substantially worsen the underlying disease, acne that progresses untreated can cause permanent scarring that no future medication will reverse.
The Future of Step-Therapy Regulation and Acne Treatment Access
As states like New Jersey implement stronger step-therapy protections, other states are likely to follow, particularly if patients and dermatological organizations continue advocating for regulatory change. The American Academy of Dermatology and other medical societies have criticized step-therapy requirements for inappropriately delaying acne treatment, arguing that insurance companies lack the clinical expertise to second-guess individual treatment decisions. Federal legislation addressing step-therapy transparency and timelines has been proposed in Congress but has not yet passed, meaning that protections will likely continue developing at the state level rather than nationally for the next several years.
In the interim, the practical reality is that dermatologists have developed more efficient exception-request processes, many now submitting requests electronically with standardized documentation that speeds approval. Some practices employ staff specifically trained in insurance prior authorization to reduce delays. For patients, understanding your insurance plan’s step-therapy requirements, asking your dermatologist about exception processes upfront, and being prepared to file an urgent request if medically necessary remains the most effective strategy for navigating these requirements.
Conclusion
Step-therapy requirements for acne are insurance cost-containment measures that force patients to try and fail cheaper medications before coverage is approved for more expensive treatments prescribed by dermatologists. While the system is designed to prevent overutilization of expensive medications, it frequently creates inappropriate delays for patients with acne severity that justifies direct treatment with specific medications. Understanding how step therapy works, knowing when to request an exception, and recognizing your rights under state-specific regulations can significantly reduce delays in accessing the medication your dermatologist has determined is necessary for your care.
If your prescription is denied due to step-therapy requirements, don’t accept the denial passively. Work with your dermatologist’s office to file a step-therapy exception request immediately, especially if you have documented reasons why the required first-step treatment is not appropriate for your case. If you’re in New Jersey or another state with step-therapy protections, reference those regulations in your request. Most exception requests are ultimately approved, but approval happens faster when dermatologists submit comprehensive documentation that directly addresses why their prescribed treatment is medically necessary.
You Might Also Like
- Why Tactupump Is Popular in Canada for Acne Treatment
- Why Winlevi Clascoterone Is Different from Other Acne Treatments
- Why Tretinoin Microsphere Is Better for Sensitive Acne Skin
Browse more: Acne | Acne Scars | Adults | Back | Blackheads