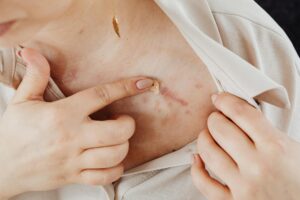
The most effective way to prevent hyperpigmentation after breakouts is to use a daily sunscreen with SPF 30 or higher—preferably SPF 50 or above if you have a history of hyperpigmentation or darker skin tones. Research shows that consistent daily sunscreen use resulted in 81% of patients noticing a lightening of pre-existing hyperpigmented marks. This isn’t just about sun protection; it’s about stopping the cascade that turns healing acne into permanent dark spots. When acne heals, inflammation triggers melanocytes to overproduce melanin as a stress response.
UV rays then act as a catalyst, signaling those pigment cells to deposit even more melanin into surrounding skin areas, creating the post-inflammatory hyperpigmentation (PIH) that can last months or years. The good news is that prevention is straightforward and starts before breakouts even appear. Beyond sunscreen, preventing hyperpigmentation requires a two-pronged approach: treating active breakouts quickly to minimize inflammation, and avoiding the single worst habit—picking or popping pimples. In this article, we’ll cover the full prevention strategy, the topical treatments that can lighten existing marks, procedural options like laser therapy, and the behavioral changes that make the biggest difference in your results.
Table of Contents
- Why Does Acne Leave Dark Spots, and How Does Sun Exposure Make It Worse?
- The Foundation of Prevention: Sunscreen and Daily Photoprotection
- Treating Breakouts Early to Reduce Inflammation
- The Most Important Prevention Step: Stop Picking and Popping Pimples
- Gentle Skincare to Minimize Additional Inflammation
- Topical Treatments for Preventing and Treating Hyperpigmentation
- Advanced Treatments and the Future of Hyperpigmentation Management
- Conclusion
Why Does Acne Leave Dark Spots, and How Does Sun Exposure Make It Worse?
Post-inflammatory hyperpigmentation happens because your skin’s healing response is overzealous. When acne inflames your skin, your body signals melanocytes—the cells that produce pigment—to step up production, thinking melanin will protect the damaged area. This is a useful mechanism in theory, but it often overshoots, leaving dark patches even after the pimple has healed. For people with deeper skin tones, this response tends to be more pronounced, which is why hyperpigmentation is a particular concern in Black, Latino, Asian, and Middle Eastern communities. UV exposure amplifies this problem significantly. Sunlight doesn’t just darken existing marks; it actively signals your melanocytes to produce more melanin.
If you’re already dealing with inflammation from a breakout, adding UV exposure on top accelerates pigment deposition. A person with active acne who spends a week at the beach without sunscreen might watch their skin darken noticeably within days. This is why dermatologists emphasize that prevention of hyperpigmentation is fundamentally about sun protection during the healing phase of acne. The timeline matters too. Hyperpigmentation can develop immediately after a pimple starts healing or emerge over weeks as inflammation subsides. Once established, PIH can persist for months or even years without treatment, though it does typically fade naturally over time (though far more slowly than with intervention). This is why the prevention approach—stopping it before it happens—is so much more effective than trying to treat it afterward.

The Foundation of Prevention: Sunscreen and Daily Photoprotection
Sunscreen should be the cornerstone of your hyperpigmentation prevention strategy, but the SPF level matters. While SPF 30 provides a baseline (blocking about 97% of UVB rays), research and dermatologists like those at Kirsch Dermatology recommend SPF 50 or higher for individuals with a history of hyperpigmentation, melasma, or those who burn quickly. Higher SPF offers protection against a broader spectrum of UV damage, and the difference between SPF 30 and SPF 50 is meaningful when your skin is prone to darkening. However, many people apply sunscreen inconsistently or in insufficient quantities, which undermines its effectiveness. The recommended amount is about one-quarter teaspoon for your face, applied every two hours (or after swimming or sweating).
Many people use half that amount, which reduces protection significantly. If you’re dealing with active acne, you also need to choose a sunscreen formulation that won’t clog your pores—a mineral sunscreen with zinc oxide or titanium dioxide is often safer than chemical sunscreens for acne-prone skin, though some people find mineral formulas too thick. The tradeoff is that mineral sunscreens can leave a white cast, especially on darker skin tones, whereas chemical sunscreens blend in better but may irritate sensitive, inflamed skin. Daily sunscreen use needs to become as automatic as brushing your teeth. This means applying it every single morning, even on cloudy days (UV rays penetrate clouds), and reapplying after sun exposure. The 81% improvement in hyperpigmentation observed in the Healthline research came from people who were consistent and diligent, not occasional users.
Treating Breakouts Early to Reduce Inflammation
The second pillar of prevention is treating active acne quickly. The American Academy of Dermatology emphasizes that treating breakouts promptly reduces inflammation, and since inflammation is the root cause of post-inflammatory hyperpigmentation, early treatment directly helps prevent PIH. This means not waiting weeks to see if a pimple will go away on its own, but instead addressing it with appropriate acne treatments—whether that’s benzoyl peroxide, salicylic acid, retinoids, or prescription options like adapalene. The reason early treatment prevents hyperpigmentation is straightforward: less inflammation means fewer signals sent to melanocytes to overproduce pigment. A pimple treated with benzoyl peroxide within a day or two will cause far less inflammatory response than one left to develop for a week.
If you’re someone prone to hyperpigmentation, this is especially critical. Your skin is signaling melanin production more aggressively than average, so every day of inflammation counts. One important caveat: using very harsh or irritating treatments in hopes of faster results can backfire. Over-drying your skin or using excessive concentrations of active ingredients can actually increase inflammation and trigger more melanin production. The goal is effective, not aggressive—use appropriate concentrations (for example, 2.5% benzoyl peroxide is as effective as 10% but less irritating) and give treatments time to work.

The Most Important Prevention Step: Stop Picking and Popping Pimples
Dr. Sandra Lee and other dermatologists identify not extracting or manipulating breakouts as the single most important preventive action to avoid post-inflammatory marks. When you pick, squeeze, or pop a pimple, you’re physically traumatizing already-inflamed skin and driving bacteria deeper, which intensifies the inflammatory response. More inflammation equals more melanin production equals darker, longer-lasting hyperpigmentation. This is harder than it sounds, especially when you have a whitehead you know could be easily drained.
But the prevention benefit is enormous. A pimple you leave alone will heal and potentially fade without a trace; a pimple you pick will almost certainly leave a mark, and if your skin is prone to hyperpigmentation, that mark may darken significantly. The comparison is stark: a pimple treated with topical acne medication and left alone might be gone in 3-5 days with minimal discoloration, whereas the same pimple extracted might take weeks to heal and leave a brown mark that lasts months. If you absolutely must address a whitehead, using a warm compress to encourage natural drainage, or visiting a dermatologist or aesthetician for professional extraction, is far safer than picking at home. Professional extraction uses sterile instruments and proper technique, minimizing trauma and subsequent inflammation.
Gentle Skincare to Minimize Additional Inflammation
How you cleanse and care for your skin while dealing with acne significantly impacts whether you’ll develop hyperpigmentation. La Roche-Posay dermatologists recommend applying a mild cleanser gently with fingertips, avoiding harsh scrubbing or pore-clogging products. Aggressive scrubbing, exfoliating brushes, or physical scrubs can aggravate acne and trigger additional inflammation—exactly what you’re trying to avoid. The limitation here is that “gentle” sometimes feels ineffective when you’re dealing with breakouts and excess oil. There’s a temptation to use harsher cleansers, thinking they’ll better address the problem.
In reality, over-cleansing or using harsh products strips your skin’s barrier, triggering reactive inflammation and sometimes making acne worse. A simple routine—gentle cleanser twice daily, appropriate acne treatment, moisturizer, and sunscreen—beats an elaborate routine with multiple harsh products. Additionally, be cautious with other skincare ingredients while you’re prone to breakouts and hyperpigmentation. Vitamin C serums, niacinamide, and other actives can be helpful, but they can also irritate inflamed skin. Layer them slowly and watch for increased redness, which signals you’re adding too much irritation on top of existing acne inflammation.

Topical Treatments for Preventing and Treating Hyperpigmentation
If prevention hasn’t fully stopped hyperpigmentation from developing, several topical treatments can help. The most promising are dual-action agents—azelaic acid, adapalene, and cysteamine cream—which have both anti-melanogenic (pigment-reducing) and anti-inflammatory properties. Azelaic acid, for example, both reduces melanin production and calms inflammation, making it particularly useful for acne-prone skin prone to hyperpigmentation.
More established options include hydroquinone (a skin-lightening agent), retinoids (which boost cell turnover and fade discoloration), and tranexamic acid. These work through different mechanisms but all help lighten existing marks. The timeframe for results is typically 8-12 weeks of consistent use. If you’re using any of these treatments, sun protection becomes even more critical—many actually increase sun sensitivity, so SPF 50+ is non-negotiable.
Advanced Treatments and the Future of Hyperpigmentation Management
For hyperpigmentation that doesn’t respond to topical treatments, procedural options exist. Low-fluence laser therapy using 1064-nm Nd:YAG laser has demonstrated the ability to completely clear post-inflammatory hyperpigmentation in published research from Wiley Online Library. These lasers work by targeting melanin without damaging surrounding skin, and results can be dramatic.
However, laser treatment requires multiple sessions (typically 3-6), costs several hundred to thousands of dollars, and carries some risk of adverse effects, particularly in darker skin tones. An emerging approach is microneedling combined with Panax ginseng-derived exosomes, which shows promise for treating post-inflammatory hyperpigmentation following acne. This combines the collagen-stimulating benefits of microneedling with growth factors from exosomes to promote faster healing and reduce discoloration. The PIH treatment market is growing rapidly—projected to expand from $1.47 billion in 2025 to $1.65 billion in 2026—reflecting both demand from patients and ongoing innovation in treatment options.
Conclusion
Preventing post-inflammatory hyperpigmentation after breakouts is entirely within your control. The strategy is straightforward: use SPF 50+ sunscreen daily, treat active breakouts quickly to minimize inflammation, resist picking or popping pimples, and maintain a gentle skincare routine. These behavioral and preventive steps will stop hyperpigmentation before it starts in most cases.
For anyone prone to hyperpigmentation, this prevention approach isn’t optional—it’s the foundation of clear, even-toned skin. If hyperpigmentation does develop despite prevention efforts, don’t despair. Topical treatments like azelaic acid, retinoids, and hydroquinone can lighten marks over time, and procedural options like laser therapy can provide dramatic results for stubborn discoloration. The key is starting early with prevention while you still can, and addressing marks promptly if they do appear rather than hoping they fade naturally, which can take a year or more.
You Might Also Like
- Why Some Skin Types Are More Prone to Hyperpigmentation
- Why Exfoliation Helps Fade Hyperpigmentation Gradually
- Why Consistency Is Key for Treating Hyperpigmentation
Browse more: Acne | Acne Scars | Adults | Back | Blackheads