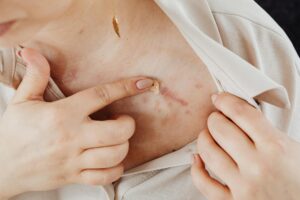
Sun exposure makes red acne marks and scars dramatically more visible because UV radiation triggers increased blood flow to the skin and intensifies existing inflammation, making pink and red discoloration appear significantly darker and more pronounced. When you spend time in the sun, especially during peak hours between 10 AM and 4 PM, the heat dilates blood vessels in the skin, and ultraviolet rays stimulate inflammatory responses that concentrate blood around damaged or healing tissue.
This is why someone with post-inflammatory erythema (PIE) or fresh acne scarring might notice their red marks look almost normal indoors but become strikingly visible at the beach or after a day outside. This article explains the biological mechanisms behind why sun exposure exacerbates red marks, how different types of acne damage respond to sunlight, practical ways to prevent this visibility increase, and what treatment options work best if you’re dealing with red marks that worsen in the sun. Understanding this relationship helps you manage expectations during treatment and make informed decisions about sun protection and when to pursue professional interventions.
Table of Contents
- Why Does Sunlight Make Red Acne Marks Appear Darker?
- The Role of Inflammation in Sun-Triggered Mark Visibility
- Sun Damage and Progressive Worsening of Red Marks
- Sun Protection Strategies That Reduce Mark Visibility
- Why Sunscreen Alone Isn’t Always Sufficient During Active Treatment
- Red Marks in Different Skin Types and Sun Scenarios
- The Future of Red Mark Treatment in Relation to Sun Exposure
- Conclusion
- Frequently Asked Questions
Why Does Sunlight Make Red Acne Marks Appear Darker?
Red acne marks consist primarily of dilated blood vessels and excess hemoglobin in the dermis—essentially, concentrated blood that shows through the skin‘s surface. When UV rays hit the skin, they damage cells and trigger an inflammatory cascade that increases blood vessel diameter and blood flow to the affected areas, which is your body’s natural healing response. This increased vascular activity makes the red marks more saturated and visually prominent because there’s more blood concentrated in those spots compared to surrounding skin. Additionally, sun exposure generates heat that naturally dilates blood vessels throughout the skin as a thermoregulation mechanism.
Someone with untreated acne marks sitting in direct sunlight will experience vasodilation specifically around areas of damage, making red marks stand out in stark contrast to normal skin tone. The effect is similar to how your face flushes when you’re embarrassed or hot—the same vasodilation is occurring, but localized to scarred or inflamed tissue. A practical example: someone with mild post-inflammatory erythema from acne might barely notice the marks indoors, but after spending two hours at a pool or beach, the marks become bright pink or red and remain noticeably darker for several hours afterward. This isn’t permanent damage from a single sun session, but rather a temporary intensification of the visible discoloration.

The Role of Inflammation in Sun-Triggered Mark Visibility
Inflammation is the core mechanism driving this process. When UV radiation penetrates the skin, it damages cellular DNA and generates reactive oxygen species (free radicals), which the body recognizes as injury. This triggers mast cells and immune cells to release inflammatory mediators like histamine and cytokines, increasing blood vessel permeability and diameter. For someone with existing acne damage, these inflamed areas are already prone to excess blood vessel activity, so sun exposure amplifies this existing inflammatory state rather than creating new inflammation from scratch.
The inflammatory response is proportional to UV dose and skin sensitivity. Fair-skinned individuals typically experience more pronounced inflammation from the same sun exposure compared to darker skin tones, which means red marks become more visually exaggerated. However, even people with darker skin experience this effect—the marks may not appear as bright red, but they shift in color and become more visible due to increased blood flow and potential hyperpigmentation from UV stimulation. One important caveat: if you’re using topical acne treatments like retinoids or chemical exfoliants, your skin’s inflammatory response to sun exposure may be significantly heightened, making red marks appear even more pronounced than they would otherwise.
Sun Damage and Progressive Worsening of Red Marks
Repeated or intense sun exposure without protection doesn’t just make red marks temporarily more visible—it can actually slow the natural fading process and make the marks more difficult to treat long-term. UV radiation damages collagen and elastin fibers in the dermis, which are essential for skin remodeling and the gradual replacement of scarred tissue with healthy skin. Each sun exposure without adequate protection potentially delays the healing timeline, meaning a mark that might have faded in 6 months with sun protection could take 12 months without it.
Additionally, chronic sun exposure can trigger increased melanin production around acne scars, leading to hyperpigmented scarring that persists long after the initial red inflammation has faded. Someone who got acne at age 16 and spent years in the sun without protection might end up with brown or gray scars rather than red ones, which are actually harder to treat with many laser and light-based therapies. For example, someone living in a sunny climate who didn’t wear sunscreen during their teenage acne years might find themselves at 25 with permanent brown post-inflammatory hyperpigmentation rather than red marks that would have naturally faded with proper sun protection.

Sun Protection Strategies That Reduce Mark Visibility
The most effective approach is combining broad-spectrum SPF 30 or higher sunscreen with physical barriers like hats and lightweight long sleeves. Broad-spectrum sunscreen blocks both UVA and UVB radiation, which are responsible for both the inflammatory response and the free radical damage that prolongs mark visibility. However, chemical and mineral sunscreens each have different implications for acne-prone skin: mineral sunscreens (zinc oxide, titanium dioxide) are less likely to clog pores but may leave a white cast on darker skin tones, while chemical sunscreens (oxybenzone, avobenzone) absorb more seamlessly but can occasionally trigger sensitivity in acne-prone or inflamed skin.
Physical barriers are often underrated but remarkably effective. Wearing a lightweight UPF-rated shirt, a wide-brimmed hat, or even sitting under a beach umbrella during peak sun hours (10 AM–4 PM) reduces UV exposure far more effectively than any sunscreen alone, since sunscreen requires reapplication and can wear off with water or sweat. The tradeoff is comfort and convenience—many people find clothing-based protection less practical than sunscreen, especially in hot weather. That said, if you’re actively treating red marks with professional treatments like laser or light therapy, dermatologists typically recommend strict physical sun avoidance for at least 48 hours post-treatment, which often means staying entirely out of direct sunlight rather than relying on sunscreen alone.
Why Sunscreen Alone Isn’t Always Sufficient During Active Treatment
Sunscreen is essential, but it’s imperfect protection. Most people apply significantly less sunscreen than the amount used in SPF testing (1/4 teaspoon per square inch of face), which means real-world protection is often closer to SPF 15 or 20 even when using SPF 50. Additionally, sunscreen degrades with sweat, water exposure, and friction, requiring reapplication every 2 hours—something most people don’t do consistently.
If you’re treating red marks with professional procedures like microneedling, laser therapy, or even prescription retinoids, the skin barrier is compromised and more vulnerable to UV damage, making sunscreen-only protection risky. A critical warning: using any acne treatment that increases skin sensitivity (retinoids, benzoyl peroxide, salicylic acid, AHAs/BHAs) without strict sun avoidance can actually worsen red mark appearance even if the treatment itself is working. The combination of treatment-induced sensitivity plus sun exposure creates excessive inflammation that negates the benefits of the treatment. Someone using prescription tretinoin for acne scarring might see better results staying indoors on sunny days than applying sunscreen and going outside, because the skin is simply too compromised to handle full sun exposure even with protection.

Red Marks in Different Skin Types and Sun Scenarios
The visibility of red marks in sunlight varies significantly based on skin tone, mark depth, and the type of damage. In fair skin, red marks show as bright pink or crimson in sunlight, making them highly visible. In medium skin tones, red marks shift toward orange-red and become less shocking but still clearly visible. In darker skin tones, red marks may appear less prominent in natural light but can become hyperpigmented or develop a purple-gray tone with sun exposure due to increased melanin production.
This doesn’t mean darker skin tones are protected—the marks are still present and worsening; they’re just visually different. The type of mark also matters. Shallow, flat post-inflammatory erythema (from surface inflammation) shows the most dramatic visibility change in sunlight, while deeper atrophic scarring (icepick or rolling scars) shows less dramatic color shifts because the discoloration is less about blood vessel concentration and more about structural loss. Someone with both red marks and depressed scarring will notice the red marks practically disappearing into the scar texture when indoors, but becoming starkly visible in sunlight—a useful indicator that treating the vascular component first (with laser or light therapy) should be prioritized.
The Future of Red Mark Treatment in Relation to Sun Exposure
Emerging treatments are specifically designed to address the vascular component of red marks without depending entirely on long-term sun avoidance. LED light therapy and newer laser systems like the 1927 nm and 1540 nm wavelengths can selectively target hemoglobin and blood vessels while minimizing melanin stimulation, meaning they’re particularly effective for people who live in sunny climates or can’t maintain strict sun protection. These technologies work better when combined with consistent sun protection, but they’re less dependent on it than older treatments.
Additionally, research into oral antioxidants and anti-inflammatory supplements suggests that internal inflammation management might reduce sun-triggered visibility increases, though evidence is still preliminary. Regardless of future advances, sun protection remains non-negotiable for anyone with red marks or active acne scarring, because the inflammatory response to UV exposure fundamentally works against healing. Even as treatments improve, preventing additional sun damage remains one of the most cost-effective interventions available.
Conclusion
Sun exposure makes red acne marks visibly darker and more pronounced through mechanisms of increased blood flow, triggered inflammation, and heat-induced vasodilation. These effects can be temporary (fading within hours of sun removal) or long-term (slowing mark fading and causing progressive hyperpigmentation), depending on the frequency and intensity of unprotected sun exposure. Understanding this relationship is crucial for anyone treating acne scarring or post-inflammatory erythema, because sun protection directly impacts treatment effectiveness and healing timeline.
If you’re dealing with red marks, prioritize broad-spectrum SPF 30+ sunscreen paired with physical barriers like hats or UPF clothing, especially during peak sun hours and while undergoing professional treatments. For marks that persist despite sun protection or don’t fade within 6–12 months, professional interventions like laser therapy or light-based treatments can accelerate healing and reduce vascular visibility. The combination of consistent sun avoidance and targeted professional treatment produces the fastest and most durable results.
Frequently Asked Questions
How long does sun-triggered redness last after going inside?
Mild redness typically fades within 1–4 hours as blood vessels normalize and inflammation subsides. Severe cases or prolonged sun exposure can leave marks visibly darker for 6–12 hours. If you’re actively treating marks with laser or light therapy, the timeline extends significantly.
Can I use sunscreen instead of avoiding sun during acne treatment?
Sunscreen is essential but incomplete protection during active acne treatment. If possible, combine sunscreen with physical barriers (hats, shade) or avoid direct sun entirely during the first 48 hours post-procedure. Prescription treatments like tretinoin require strict sun avoidance for optimal results, not just sunscreen application.
Do red marks ever fade without treatment if I protect from sun?
Yes. Post-inflammatory erythema typically fades within 6–12 months with consistent sun protection and no additional irritation. Deeper atrophic scarring won’t improve without professional treatment, but sun protection prevents the marks from worsening or developing hyperpigmentation that’s harder to treat later.
Why do my red marks look worse after swimming even with waterproof sunscreen?
Waterproof sunscreen degrades with water immersion, chlorine, and friction—you’re likely receiving less protection than expected. Additionally, heat from sun exposure plus water temperature increases vasodilation and inflammation simultaneously. Consider swimming in early morning or late afternoon, or wearing a UPF-rated rash guard instead.
Is laser treatment more effective than waiting with sun protection?
Laser therapy accelerates results significantly—marks that might take 12+ months to fade with sun protection alone typically show substantial improvement in 3–6 months with professional treatment. However, laser requires strict sun protection post-procedure, so the treatment itself doesn’t eliminate the need for sun avoidance.
You Might Also Like
- Why Sensitive Skin Is More Prone to Post Acne Red Marks
- What Makes Red Acne Marks Different From Pigmentation
- What Happens Under the Skin When Red Marks Appear After Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads