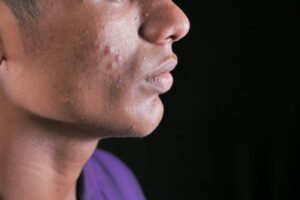
When you combine too many redness treatments at once, you risk damaging your skin barrier, reducing the effectiveness of active ingredients, and triggering severe irritation or allergic reactions. For example, if you’re using benzoyl peroxide in the morning and retinol at night while also taking oral doxycycline, the benzoyl peroxide will deactivate the retinol, your skin may become overly sensitized, and you’ll experience side effects without getting the benefits you expected. The problem is that most people with persistent redness—whether from acne, rosacea, or inflammation—want to solve the problem as quickly as possible, so they layer multiple treatments hoping for faster results.
This article explains what actually happens when you overdo it, which combinations are particularly dangerous, how to space treatments safely, and when you need medical guidance. Dermatologists have clear evidence that more treatment doesn’t equal better results. In fact, the opposite is usually true: adding too many active ingredients overwhelms your skin’s ability to adapt and repair itself. Understanding the specific conflicts between common redness treatments is the first step to building a routine that actually works.
Table of Contents
- Why Mixing Multiple Redness Treatments Backfires
- How Over-Exfoliation Damages the Skin Barrier
- Acne Treatments Are Not Suitable for Rosacea-Prone Skin
- Spacing Treatments Several Weeks Apart Is Essential
- Oral Medications Create Additional Complications
- Recognizing When Your Skin Is Telling You to Stop
- Building a Sustainable Redness Treatment Plan
- Conclusion
Why Mixing Multiple Redness Treatments Backfires
The core issue is that redness treatments work through different mechanisms, and when you combine them incorrectly, they interfere with each other or create compounding irritation. Benzoyl peroxide is an oxidizing agent commonly used for acne-related redness, while retinol is a vitamin A derivative that reduces inflammation and promotes cell turnover. When you use benzoyl peroxide and retinol in the same routine (or even on the same day), the benzoyl peroxide chemically deactivates the retinol before it can do its job. You’re essentially canceling out the retinol’s benefits while increasing the irritation risk from both ingredients.
The timing issue becomes even more critical when you add a third or fourth treatment. If you’re also using an exfoliating acid like salicylic acid or glycolic acid, you’re now weakening your skin barrier from multiple angles simultaneously. Your skin can tolerate some degree of exfoliation, some degree of retinization (the adjustment period to retinol), and some degree of benzoyl peroxide oxidation—but not all at once. The safe approach is separating these treatments: benzoyl peroxide in the morning, retinol at night, with exfoliating acids used only a few times per week, not daily.

How Over-Exfoliation Damages the Skin Barrier
Your skin barrier is a protective layer that keeps water in and irritants out. When you use multiple exfoliating treatments—whether they’re chemical exfoliants (acids, retinoids) or physical exfoliants (scrubs, brushes)—too aggressively or simultaneously, you strip away this barrier. The result is compromised skin: it becomes drier, peels more visibly, and becomes hypersensitive to almost everything you apply, including treatments that should be helping. The damage from over-exfoliation can persist for weeks, even after you stop using the irritating products.
You might notice increased sensitivity, a rough or sandpaper-like texture, persistent redness that won’t improve, or a stinging sensation when you apply even gentle products. However, if your redness is mainly from dryness caused by over-exfoliation, adding more active treatments will worsen it. This is where many people get stuck in a cycle: they develop barrier damage, their skin gets redder and more sensitive, they assume they need stronger treatments, and they end up making the problem worse. Breaking this cycle requires stopping the excess treatments and allowing your barrier to heal, which can take 2-4 weeks depending on severity.
Acne Treatments Are Not Suitable for Rosacea-Prone Skin
One of the most common dangerous combinations is using acne treatments on rosacea-prone skin. Acne vulgaris treatments like salicylic acid and retinol are designed to aggressively exfoliate and promote cell turnover. On typical acne-prone skin, this works well. But rosacea-prone skin is inherently more sensitive and reactive, and these harsh treatments often trigger or worsen rosacea symptoms rather than improving them. If you have rosacea or rosacea-like sensitivity, acne treatments can push your condition from manageable to severe.
This distinction matters because many people with redness assume they have acne when they actually have rosacea, or they have both conditions simultaneously. The treatments for acne vulgaris and rosacea are completely different, and using the wrong one can backfire significantly. If you’re combining benzoyl peroxide (for acne), azelaic acid (also often used for acne), sulfur products, or strong retinoids while also having underlying rosacea, you’re essentially fighting your own skin. The American Academy of Dermatology notes that acne treatment products are too harsh for rosacea-prone skin and can worsen rosacea symptoms when applied to sensitive skin. Before combining any redness treatments, you need to know whether you’re dealing with acne, rosacea, post-inflammatory hyperpigmentation, or a combination—because the approach is very different.
Spacing Treatments Several Weeks Apart Is Essential
Dermatologists recommend spacing multiple treatments several weeks apart, not days or even one week apart. This gives your skin time to fully respond to each treatment before you introduce the next variable. When you’re trying a new redness treatment, you should use it consistently for 2-4 weeks before adding another treatment. This allows you to assess whether it’s actually working and whether your skin is adapting well. The practical strategy is to introduce treatments one at a time on a rotation.
For example: Week 1-4, use benzoyl peroxide in your morning routine to see how your skin responds. After 4 weeks, if your skin has adjusted well, add retinol 2-3 times per week in your evening routine. After another 3-4 weeks, if you still have redness and your skin is tolerating both treatments, you might add an azelaic acid treatment 2-3 times per week. The comparison is useful here: adding one treatment every 4 weeks means you’ll have a properly assessed routine in 3-4 months, versus adding three treatments at once and having no idea which one is causing the irritation or which one is actually helping. Patience yields better results and fewer setbacks.
Oral Medications Create Additional Complications
If you’re taking oral medications for redness—like doxycycline for rosacea or acne, or other antibiotics—you need to be especially careful about what topical treatments you combine them with. Doxycycline has notable side effects: approximately 10 out of 100 people experience diarrhea, nausea, and photosensitivity (increased sensitivity to sun exposure). If you’re also using multiple topical actives like retinol, benzoyl peroxide, and exfoliating acids, you’re compounding the irritation and photosensitivity risk. The warning here is that topical treatments don’t exist in isolation from your oral medications.
Metronidazole, another common treatment for rosacea and certain types of acne, has its own topical side effects including itching, stinging, irritated skin, and dryness at application sites. Adding multiple exfoliating or drying topical treatments on top of metronidazole frequently results in severe dryness, flaking, and a damaged barrier. Before combining any topical treatments, you must consult with your dermatologist about your current oral medications, dosages, and potential drug interactions with anything else you’re taking. What seems like a reasonable topical routine might not be safe given your specific medication profile.

Recognizing When Your Skin Is Telling You to Stop
Your skin provides clear signals when you’ve combined too much. Persistent stinging or burning, even with gentle cleansers, means your barrier is compromised. Increased redness rather than improvement is a sign that your treatments are irritating rather than healing. Visible peeling, flaking, or a sandpaper texture indicates barrier damage.
Unexplained breakouts or pustules in areas where you usually don’t break out can signal that your combination of treatments has triggered a reaction or shifted your skin’s microbiome. If you notice any of these signs, the first step is to stop everything except a gentle cleanser, hydrating moisturizer, and sunscreen for 2-4 weeks. This sounds counterintuitive—stopping treatment when you want results—but it’s the only way to let your barrier recover. Many people misinterpret these warning signs as a reason to add more treatment (thinking they’re not being aggressive enough), which deepens the damage. Once your skin has healed and stabilized, you can reintroduce treatments one at a time, much more slowly and conservatively than before.
Building a Sustainable Redness Treatment Plan
Working with a dermatologist before combining treatments is the most reliable way to avoid these problems. Your dermatologist can identify your specific type of redness, assess your skin’s tolerance for actives, review your current medications, and create a plan that’s tailored to you rather than generic. What works for someone with mild acne-related redness will be very different from what works for someone with rosacea or post-inflammatory erythema.
As you move forward, remember that the goal is sustained improvement over months, not dramatic results in weeks. A slow, methodical approach—one treatment introduced every 4 weeks, each one separated by timing or formulation, and each one backed by your dermatologist’s approval—produces better long-term outcomes than an aggressive approach that damages your barrier. The most effective skincare routine is one your skin can tolerate indefinitely, not one that creates a crisis and forces you to stop everything.
Conclusion
Combining too many redness treatments overwhelms your skin’s ability to repair and adapt, resulting in barrier damage, reduced efficacy of individual treatments, and often worse redness rather than improvement. The specific conflicts—like benzoyl peroxide deactivating retinol, acne treatments triggering rosacea, or over-exfoliation compromising your barrier—are avoidable with proper spacing, timing, and medical guidance. Dermatologists recommend introducing treatments several weeks apart, using different formulations at different times of day, and checking in regularly to assess tolerance.
Your next step is to audit your current routine: identify every active treatment you’re using, the timing, and how long you’ve been using them. If you’re using more than two active treatments simultaneously, you’re likely overdoing it. Schedule a consultation with a dermatologist before adding anything new, discuss your specific type of redness and your treatment goals, and follow their recommendation for spacing and combinations. The fastest way to results is not the most aggressive routine—it’s the routine that works with your skin’s biology rather than against it.
You Might Also Like
- Why Some Treatments Make Redness Worse Before It Improves
- What Happens When Your Skin Becomes Resistant to Acne Treatments
- What Happens When You Treat Redness Like Acne
Browse more: Acne | Acne Scars | Adults | Back | Blackheads