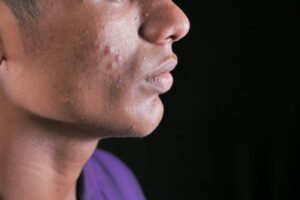
Some people sail through their teenage years with clear skin, only to be blindsided by acne breakouts in their 20s, 30s, or beyond. This happens because acne is fundamentally driven by genetic predisposition that can remain dormant during adolescence and activate later in life—especially when triggered by hormonal shifts, stress, or lifestyle changes unique to adulthood. While genetics load the gun, hormonal fluctuations and environmental factors pull the trigger, which is why two people with similar genetic backgrounds can experience acne at completely different life stages. This article explores why late-onset acne affects millions of adults who breezed through their teenage years, examines the primary mechanisms behind delayed acne development, and covers the most effective treatment options available today.
Table of Contents
- Why Genetic Predisposition Doesn’t Always Show Up in Teenage Years
- Hormonal Changes as the Primary Trigger for Adult-Onset Acne
- The Adult Acne Gender Divide and Its Implications
- Environmental and Lifestyle Triggers Emerging in Adulthood
- Medical Conditions and Systemic Factors Unique to Adulthood
- The Role of Persistent Versus Late-Onset Acne in Treatment Planning
- Recent Advances in Adult Acne Treatment and Future Outlook
- Conclusion
Why Genetic Predisposition Doesn’t Always Show Up in Teenage Years
acne has a strong genetic component—twin studies from the UK show that approximately 81% of acne cases carry a genetic element. Yet having the genes that predispose you to acne doesn’t guarantee you’ll develop it as a teenager. Genetic vulnerability acts as a loaded foundation, but it requires specific environmental and biological conditions to activate. For some people, those conditions never materialize during puberty, only to emerge in early adulthood or middle age.
This is why you might have a parent or sibling with teenage acne while you had clear skin at 16, then developed acne at 25. The genetics were always there; the circumstances that trigger their expression simply weren’t present when you were younger. The delay in manifestation highlights an important distinction: genetic predisposition is necessary but not always sufficient for acne to develop. Someone with acne genes might never show symptoms if they avoid trigger factors, or their triggers might not activate until hormonal conditions shift significantly—such as when entering the workforce, experiencing chronic stress, or undergoing hormonal changes related to reproductive health.
Hormonal Changes as the Primary Trigger for Adult-Onset Acne
Hormonal fluctuations represent the dominant factor in adult-onset acne, particularly for women. Androgen hormones—specifically testosterone and its derivatives—are the main drivers of acne in adults, which is why inhibiting androgen production is key to achieving sustained clear skin. During adolescence, everyone experiences surging androgens that can trigger acne in genetically susceptible individuals. However, many teenagers with acne genes don’t develop breakouts during puberty due to other protective factors or simply being genetically less sensitive to androgens at that age. Fast forward to adulthood, and hormonal patterns change.
Women may experience irregular menstrual cycles, develop polycystic ovary syndrome (PCOS)—which is the primary endocrinological cause of adult female acne—or undergo shifts related to pregnancy, oral contraceptive use, or perimenopause. These hormonal events can unmask a latent genetic predisposition. However, if you’re genetically resistant to androgen-driven acne, simply having elevated androgens as an adult won’t necessarily trigger breakouts. The key mechanism involves both genetic vulnerability and androgen sensitivity colliding—which explains why some women with PCOS develop severe cystic acne while others with similar hormone profiles remain clear. Hormonal therapies, particularly combined oral contraceptives, work by suppressing ovarian androgen production and increasing sex hormone-binding globulin (SHBG), which makes androgens less biologically available. This treatment approach specifically targets the adult-acne mechanism and is why hormonal therapy remains the primary treatment for women with adult-onset acne.
The Adult Acne Gender Divide and Its Implications
Adult acne presents a strikingly different demographic pattern than teenage acne. While adolescent acne affects males and females relatively equally, approximately 73.8% of adult acne patients are women—a dramatic shift compared to 64.55% in adolescent acne. This disparity directly reflects the hormonal nature of late-onset breakouts. Women’s reproductive-related hormonal changes create multiple windows of vulnerability that don’t exist in adolescent boys the same way.
Additionally, about 50% of adult acne patients report a familial history of adult-onset acne, suggesting that some families carry not just a genetic predisposition to acne generally, but specifically to the late-manifesting form. The female dominance in adult acne also creates a practical reality: treatment guidelines and research increasingly focus on hormonal approaches, which have limited applicability for men with adult-onset acne. Men developing acne in their 30s or 40s typically have different underlying causes—often related to topical irritants, harsh skincare, occupational exposures, or systemic medications—rather than the androgen-driven mechanism seen in women. Understanding your sex matters for diagnosis and treatment selection.

Environmental and Lifestyle Triggers Emerging in Adulthood
While genetics and hormones set the stage, environmental triggers specific to adult life often activate late-onset acne. Workplace stress was cited as a precipitating factor in 50% of surveyed women with adult acne—a type of chronic psychological stress far less common in teenagers. Stress elevates cortisol, which can amplify androgen production and impair skin barrier function, creating ideal conditions for acne development. Additionally, the skincare and cosmetic products adults use are often more complex than teenage routines. Certain sunscreens, heavy moisturizers, foundations, and makeup formulations can trigger acne in genetically susceptible adults.
Topical corticosteroid misuse—sometimes resulting from using products not originally intended for the face—is another distinctly adult trigger that can provoke severe acne flares. Diet, tobacco use, and smoking represent additional adult-specific triggers that don’t apply equally across age groups. Some adults develop acne after smoking cessation (paradoxically, as skin begins detoxifying), while others find that refined carbohydrates and dairy worsen their breakouts. These triggers require time to accumulate or to be adopted as habits, which explains why someone with clear teenage skin might develop acne after years of poor sleep and high stress in their career. The key distinction: teenagers have simpler exposure profiles, while adults navigate a complex environment of potential triggers that weren’t present at age 14.
Medical Conditions and Systemic Factors Unique to Adulthood
Several systemic conditions emerging in adulthood can trigger acne in genetically predisposed individuals. Polycystic ovary syndrome (PCOS), metabolic syndrome, and autoimmune thyroiditis all show associations with adult acne development. These are conditions that typically develop gradually over time or emerge after adolescence, creating a window where acne was previously absent but now appears coincident with the underlying disorder.
For instance, a woman might have perfectly clear skin at 20, then develop PCOS in her late 20s or early 30s, with acne appearing as an early sign of the condition alongside irregular periods and metabolic changes. One important limitation: not everyone with PCOS develops acne, and not all adult acne is driven by PCOS or metabolic dysfunction. Some cases remain purely genetic-hormonal in nature without any detectable systemic disease. However, if you develop acne suddenly in adulthood alongside other symptoms like irregular cycles, weight changes, or fatigue, screening for underlying endocrine or metabolic conditions is warranted.

The Role of Persistent Versus Late-Onset Acne in Treatment Planning
A critical distinction exists between persistent acne (acne that continues from teenage years into adulthood, affecting 73.2% of adult acne patients) and true late-onset acne (first appearing in adulthood, affecting 26.8% of adult acne cases). This matters because the two types often respond differently to treatment. Persistent acne typically involves longer-standing skin inflammation and potentially deeper sebaceous gland involvement, while late-onset acne may be more responsive to hormonal intervention since hormonal shifts are often the primary recent trigger.
Someone with late-onset acne at 28 might clear completely on hormonal therapy, whereas someone with persistent acne since age 14 might require combination approaches including retinoids and hormonal treatment. This distinction also affects how dermatologists approach diagnosis. If you develop acne suddenly in your 30s, the immediate question becomes: what changed recently? Hormones, stress, skincare products, medication, or systemic health? For persistent acne patients, the question is different: why is it still present despite years of treatment, and what approach hasn’t been tried?.
Recent Advances in Adult Acne Treatment and Future Outlook
Recent advances in adult acne treatment have moved beyond older approaches, particularly with the approval of clascoterone cream 1%—the first topical androgen receptor inhibitor approved for acne in patients 12 years and older. This medication directly targets androgen signaling in skin without systemic effects, offering a new option for patients who can’t or won’t use hormonal contraceptives. Clascoterone represents a shift toward more targeted, mechanism-based treatment for adult acne rather than one-size-fits-all approaches.
As understanding of the adult acne phenotype deepens, treatments specifically designed for hormonal late-onset cases continue to evolve. The trajectory suggests future treatments will become increasingly personalized based on acne phenotype (hormonal versus non-hormonal, inflammatory markers, microbiome status) and individual genetic risk factors. For now, the most effective approach for most adults with late-onset acne remains hormonal therapy for women and comprehensive lifestyle modification combined with topical retinoids or other standard agents for both sexes.
Conclusion
Late-onset acne develops because genetic predisposition can remain dormant until adulthood, when hormonal shifts, stress, medical conditions, and environmental triggers align to activate it. The fact that you had clear teenage skin doesn’t mean you’re immune to acne—it simply means the biological and environmental circumstances required to trigger your genetic vulnerability hadn’t occurred yet. For women especially, adulthood brings multiple hormonal windows including PCOS development, menstrual irregularities, and medication changes that can unmask latent acne susceptibility in ways that don’t apply to teenagers.
If you’ve developed acne as an adult, the most productive approach involves identifying your specific triggers—whether hormonal, stress-related, or environmental—and addressing the mechanism rather than just the surface symptoms. For hormonal late-onset acne, particularly in women, hormonal therapies or newer medications like clascoterone offer targeted solutions. Consulting a dermatologist who understands adult acne’s distinct nature will help move you toward sustained clear skin faster than generic acne approaches designed primarily for teenagers.
You Might Also Like
- Why Your Acne Routine Is Not Working Even If You Follow It Consistently
- Why Your Acne Leaves Marks Even When You Do Not Pick Your Skin
- Why Some Acne Leaves Red Marks Instead of Dark Spots and What It Means
Browse more: Acne | Acne Scars | Adults | Back | Blackheads