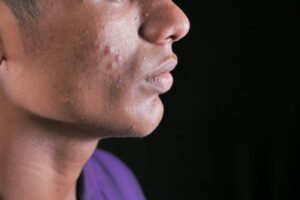
When your skin becomes resistant to acne treatments, it means the bacteria causing breakouts—particularly *Cutibacterium acnes*—has adapted to survive the medication you’ve been using. This happens because acne-causing bacteria develop genetic mutations and other survival mechanisms that allow them to thrive even when exposed to antibiotics or topical treatments repeatedly. The result is the same frustrating cycle: your acne clears for a while, then comes roaring back despite continued treatment. This resistance doesn’t mean you’re stuck with acne forever, but it does mean your dermatologist needs to switch strategies, often combining different medications or moving away from antibiotics entirely.
The problem is widespread and growing. About 30 to 50 percent of acne-causing bacteria in most developed countries are now resistant to at least some antibiotics. For some drugs like topical macrolides, resistance rates exceed 50 percent in many parts of the world. This article explains how treatment resistance develops, why it’s becoming such a common problem, what mechanisms bacteria use to survive your medications, and most importantly, what effective alternatives exist when your current treatment stops working.
Table of Contents
- How Antibiotic Resistance Develops During Acne Treatment
- The Scale of Antibiotic Resistance in Dermatology
- The Biological Mechanisms Behind Bacterial Resistance
- Why Combined Therapy Works Better Than Antibiotics Alone
- What Dermatologists Get Wrong About Long-Term Antibiotic Use
- Alternative Treatments When Resistance Develops
- The Future of Acne Treatment Without Antibiotics
- Conclusion
How Antibiotic Resistance Develops During Acne Treatment
Antibiotic resistance in acne develops through a straightforward biological process. When you take an antibiotic—whether oral doxycycline, minocycline, or a topical erythromycin—the drug kills most of the *Cutibacterium acnes* bacteria on your skin. However, a small percentage of bacteria survive because they naturally carry genes that make them resistant to that particular drug. These survivors reproduce, and over time, the resistant population grows. Eventually, the resistant bacteria outnumber the sensitive ones, and your antibiotic becomes ineffective.
This is why dermatologists now warn that using the same antibiotic for months on end accelerates resistance. The timing matters significantly. Studies show that nearly 20 percent of acne patients have been continuously prescribed oral antibiotics for more than 6 months—far exceeding the recommended 3 to 4 month maximum. Each additional month of antibiotic use increases the likelihood that resistant bacteria will dominate your skin’s microbiome. It’s not that the antibiotic suddenly stops working overnight; rather, resistance builds gradually as susceptible bacteria die off and resistant strains multiply. The longer you use an antibiotic, the more certain it becomes that you’ll eventually need to switch treatments.

The Scale of Antibiotic Resistance in Dermatology
The prevalence of antibiotic-resistant acne bacteria is staggering. In dermatology practices, approximately 54 percent of all acne prescriptions involve oral or topical antibiotics. This means antibiotics account for roughly 66 percent of all antibiotic use in dermatology—acne treatment is the primary driver. Given that acne affects approximately 85 percent of adolescents and young adults worldwide, and more than 1 billion people globally have acne, this translates to hundreds of millions of people exposed to antibiotics each year for acne treatment alone.
The consequences extend beyond individual patients. A 2018 survey of Turkish dermatologists and family physicians found that 88.5 percent of dermatologists and 79.5 percent of family physicians expressed serious concerns over antibiotic resistance in acne treatment. This isn’t a theoretical worry—it’s already affecting clinical practice. Doctors report switching antibiotics more frequently, prescribing combination therapies instead of monotherapy, and encountering patients whose acne no longer responds to standard treatments. The global antimicrobial resistance burden is estimated at approximately 4.95 million deaths associated with antimicrobial resistance in 2019, a figure that includes complications from resistant acne bacteria when infections worsen or spread.
The Biological Mechanisms Behind Bacterial Resistance
Bacteria don’t develop antibiotic resistance through willpower or adaptation in the Darwinian sense—the resistance is encoded in their DNA. The main mechanisms involve genetic mutations that modify three key components of the bacterial cell. First, some bacteria develop altered ribosomal RNA, which prevents antibiotics like tetracyclines and macrolides from binding and interfering with protein synthesis. Second, bacteria can modify their efflux pumps—cellular structures that normally accumulate antibiotics inside the cell. When these pumps are altered, they actively pump the antibiotic out before it can damage the bacteria. Third, some bacteria produce enzymes that chemically inactivate the antibiotic before it can work.
Beyond individual genetic changes, bacteria employ a sophisticated survival strategy called biofilm formation. Biofilms are communities of bacteria embedded in a protective matrix of self-produced slime. This biofilm acts as a physical barrier that reduces antibiotic penetration and allows bacteria to communicate and share resistance genes with neighbors. Once a biofilm forms on your skin, treating the acne becomes dramatically harder because antibiotics can’t reach many of the bacteria inside the protected community. This is why someone might experience acne that seems to clear but never fully resolves—biofilms can persist even when surface bacteria appear to be eliminated. The bacteria inside the biofilm also exchange genetic material with each other, spreading resistance genes throughout the community.
Why Combined Therapy Works Better Than Antibiotics Alone
The research is clear: using an antibiotic alone to treat acne is less effective and speeds up resistance compared to combining the antibiotic with a second agent like benzoyl peroxide or a retinoid. When you combine treatments, each medication targets acne through a different mechanism. Benzoyl peroxide kills bacteria directly and prevents biofilm formation. Retinoids reduce sebum production and prevent bacteria from multiplying. Antibiotics attack the remaining bacteria from a different angle. Together, these create multiple obstacles that bacteria must overcome simultaneously, making resistance far less likely to develop.
Here’s the crucial part: benzoyl peroxide has no reported resistance. Despite decades of use, bacteria have never evolved a way to survive benzoyl peroxide exposure. This is why dermatologists increasingly recommend pairing antibiotics with benzoyl peroxide, at least initially. By combining the two, you get the fast-acting bacterial kill from the antibiotic while the benzoyl peroxide prevents resistant bacteria from gaining a foothold. If resistance does eventually develop to the antibiotic, the benzoyl peroxide continues working. Studies and updated guidelines from the American Academy of Dermatology now emphasize this combination approach over antibiotic monotherapy, particularly for longer-term acne management.
What Dermatologists Get Wrong About Long-Term Antibiotic Use
A significant gap exists between best practices and actual clinical practice. Guidelines clearly state that antibiotics should be limited to a maximum of 3 to 4 months, yet nearly one in five acne patients are prescribed oral antibiotics continuously for more than 6 months. Why does this happen? Sometimes it’s because the antibiotic appears to be working reasonably well, and both doctor and patient want to avoid trying something new. Sometimes doctors aren’t aware of the current resistance statistics or haven’t updated their practice in line with newer guidelines. Sometimes patients request to stay on the same medication because they fear trying alternatives. Whatever the reason, this extended use accelerates resistance development and sets patients up for treatment failure.
The irony is that continuing an antibiotic beyond 3 to 4 months often makes your acne worse, not better. As resistance develops, the antibiotic becomes less effective, but you keep using it because you don’t immediately realize it’s stopped working. Meanwhile, resistant bacteria are proliferating. Eventually, you notice the medication isn’t working anymore, but by then you’ve been on antibiotics for eight months, nine months, or longer. At that point, switching treatments becomes necessary anyway, but you’ve lost several months where a different approach could have been more effective. Current evidence-based practice recommends reassessing treatment every 3 months and switching strategy if needed, rather than continuing indefinitely.
Alternative Treatments When Resistance Develops
When antibiotic resistance becomes apparent, several effective alternatives exist. Retinoids like tretinoin and adapalene work through entirely different mechanisms—they regulate cell turnover, reduce sebum production, and kill bacteria indirectly by creating an inhospitable environment. Unlike antibiotics, bacteria cannot develop resistance to retinoids because the drugs don’t attack the bacterial cell directly. Benzoyl peroxide, as mentioned, remains effective and can be used indefinitely without resistance concerns. Azelaic acid attacks bacteria while also reducing inflammation and evening out skin tone.
Salicylic acid and other chemical exfoliants work by clearing pores, preventing bacterial overgrowth. For moderate to severe acne, oral isotretinoin (Accutane) is the gold standard when resistance is widespread or other treatments fail. This is a potent medication with significant side effects and strict monitoring requirements, but it essentially resets the skin and can provide long-term clearance. Hormonal treatments like birth control pills or spironolactone work particularly well for hormone-driven acne. The key is that these alternatives don’t rely on antibiotic resistance mechanisms, so they remain effective regardless of what bacteria your skin harbors.
The Future of Acne Treatment Without Antibiotics
The dermatology community is slowly shifting away from antibiotic-centric acne treatment, driven by resistance data and updated guidelines. This shift is actually positive because it’s pushing innovation in non-antibiotic directions. Research is exploring probiotic approaches that introduce beneficial bacteria to compete with *Cutibacterium acnes*.
Others are investigating novel compounds that disrupt bacterial biofilm formation or target specific virulence factors without requiring resistance-prone killing mechanisms. Some dermatologists are revisiting combination strategies using multiple non-antibiotic agents from the start, which was largely abandoned in favor of antibiotics decades ago. This transition won’t happen overnight, and antibiotics will likely remain part of acne treatment for years to come. However, the mindset is changing from “prescribe an antibiotic and maintain it indefinitely” to “use an antibiotic briefly as part of a combination strategy, then transition to long-term non-antibiotic maintenance.” This approach protects both individual patients—by preventing resistance in their personal microbiome—and public health by reducing overall antibiotic consumption and slowing the development of population-level resistance.
Conclusion
When your skin becomes resistant to acne treatments, it reflects a biological reality: bacteria have evolved survival mechanisms that your current medication can no longer overcome. This resistance develops most rapidly with long-term antibiotic monotherapy, which is why current guidelines recommend limiting antibiotics to 3 to 4 months and using them as part of combination therapy rather than as standalone treatments. The good news is that resistance is not an irreversible dead end. Benzoyl peroxide, retinoids, azelaic acid, and other non-antibiotic treatments remain effective because bacteria cannot develop resistance to them.
The best strategy is prevention through informed treatment. Work with your dermatologist to use antibiotics briefly and appropriately, combine them with benzoyl peroxide or other agents, and transition to non-antibiotic maintenance therapy within the recommended timeframe. If resistance does develop, multiple effective alternatives exist. By understanding how resistance develops and following evidence-based treatment principles, you can maintain control of acne without contributing to the growing public health crisis of antibiotic-resistant bacteria.
You Might Also Like
- What Happens When You Overuse Acne Treatments and Damage Your Skin Barrier
- What Happens When Acne Becomes a Long Term Skin Condition
- What Works Better for Red Acne Marks Laser Treatments or Topical Products
Browse more: Acne | Acne Scars | Adults | Back | Blackheads