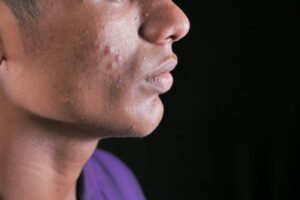
Pimples that refuse to heal and instead evolve into persistent skin issues like dark spots, pitted scars, or enlarged pores can turn a simple breakout into a long-term skincare nightmare. While most acne lesions resolve without issue, certain pimples linger due to disrupted healing processes triggered by inflammation, bacterial overgrowth, and poor wound repair in the skin. This matters because up to 80% of people experience some form of acne scarring, affecting self-confidence and requiring targeted interventions beyond basic spot treatments.
In this article, you'll learn the precise mechanisms behind why some pimples transform into lasting problems, from pore blockages and bacterial invasions to hormonal influences and picking habits. Drawing from dermatological insights, we'll break down the science of acne progression, risk factors, and prevention strategies tailored for acne-prone skin. Armed with this knowledge, you can intervene early to promote healing and minimize damage.
Table of Contents
- Why Do Some Pimples Fail to Heal Normally?
- What Turns Inflammation Into Permanent Scarring?
- Key Risk Factors That Prolong Acne Lesions
- Types of Long-Lasting Skin Problems from Pimples
- The Science of Skin Repair Gone Wrong
- How to Apply This
- Expert Tips
- Conclusion
- Frequently Asked Questions
Why Do Some Pimples Fail to Heal Normally?
Acne starts innocently when hair follicles clog with excess sebum, dead skin cells, and bacteria, forming comedones that may erupt into inflamed pimples. In healthy healing, the body's inflammatory response clears the blockage, and skin cells regenerate to close the wound seamlessly. However, when the follicle wall ruptures deeply—a process called rupture into the dermis—the contents spill into surrounding tissue, provoking intense inflammation that disrupts normal repair.
This rupture often stems from unchecked bacterial growth, particularly Propionibacterium acnes (now Cutibacterium acnes), which thrives in oil-rich, clogged pores and triggers swelling, redness, and pus formation. If inflammation persists, it damages collagen and elastin fibers essential for skin structure, leading to atrophic scars (pits) or hypertrophic scars (raised tissue). Hormonal surges amplify sebum production, making pores more prone to severe blockages that resist resolution.
- Excess sebum from androgen hormones enlarges oil glands, creating a sticky environment where dead keratinocytes cling instead of shedding, trapping bacteria.
- Bacterial proliferation in the plugged follicle causes immune overreaction, spilling inflammatory debris into deeper skin layers.
- Delayed clearance of inflammation prevents fibroblast activity, halting collagen remodeling needed for smooth healing.
What Turns Inflammation Into Permanent Scarring?
Prolonged inflammation is the pivotal shift from pimple to scar, as cytokines and enzymes degrade the extracellular matrix during aggressive immune responses. Nodular or cystic acne, characterized by deep, painful lesions, is especially scarring because they form below the skin's surface, rupturing follicles extensively and causing widespread tissue loss.
Factors like genetics influence scar formation; those with a family history of acne inherit thinner dermal layers or inefficient wound healing, making pits more likely. Picking or squeezing exacerbates this by introducing more trauma, widening the lesion, and promoting fibrosis or hyperpigmentation as melanin overproduces during repair.
- Genetic predisposition leads to excess sebum and sensitive follicles, prolonging inflammatory phases.
- Mechanical trauma from popping forces debris deeper, converting superficial pimples into ice-pick or boxcar scars.
Key Risk Factors That Prolong Acne Lesions
Hormonal fluctuations, common in adult acne, sustain oil overproduction and pore clogging, turning transient pimples into chronic issues. Stress elevates cortisol, which boosts androgens and inflammation, while diets high in dairy or glycemic foods spike insulin, indirectly fueling sebum and bacterial growth.
Environmental irritants like pollution or humidity trap sweat and oil, worsening blockages, and comedogenic products (oily moisturizers, makeup) mimic natural clogs. Medications such as steroids or lithium can mimic these effects, delaying healing.
- Hormonal events like menstruation, PCOS, or menopause increase androgen-driven sebum, leading to persistent nodules.
- Stress and high-GI diets promote systemic inflammation, slowing lesion resolution.

Types of Long-Lasting Skin Problems from Pimples
When pimples scar, they manifest as atrophic scars—ice pick (narrow pits from deep rupture), boxcar (wide depressions with sharp edges), or rolling (wavy indents from tethered tissue)—due to collagen loss in the dermis. Hypertrophic or keloid scars, more common in darker skin tones, arise from excess collagen deposition post-inflammation. Post-inflammatory hyperpigmentation (PIH) appears as flat brown or red marks from melanin overload during healing, lasting months without intervention.
Enlarged pores result from weakened follicle walls stretched by cysts, creating a textured, uneven surface. These issues persist because acne disrupts the skin's barrier, inviting secondary infections or irritation that hinder regeneration. Early treatment with retinoids or antibiotics can prevent progression, but untreated severe acne guarantees visible remnants.
The Science of Skin Repair Gone Wrong
Skin healing follows phases: hemostasis, inflammation, proliferation, and remodeling. In acne, excessive inflammation skips efficient proliferation, where fibroblasts should rebuild collagen.
Instead, matrix metalloproteinases (MMPs) from bacteria and neutrophils break down dermal scaffolding, leaving depressions. Genetics and age factor in; younger skin heals faster via robust collagen, but adult acne sufferers often face delayed remodeling due to hormonal interference. Chronic low-grade inflammation from unresolved bacteria maintains a cycle, preventing full barrier restoration.
How to Apply This
- Assess pimples daily: If red, painful, or larger than 5mm after 48 hours, apply topical benzoyl peroxide (2.5-5%) to kill bacteria and reduce inflammation without picking.
- Introduce non-comedogenic routines: Cleanse twice daily with salicylic acid (2%) to exfoliate dead cells, followed by lightweight, oil-free moisturizer and broad-spectrum SPF 30+ to protect healing tissue.
- Avoid triggers: Track diet for dairy/high-GI foods, manage stress via sleep/exercise, and switch to mineral-based makeup tested for non-comedogenicity.
- Seek professional care early: For nodules or scars-in-progress, consult a dermatologist for retinoids, chemical peels, or lasers to halt progression and stimulate collagen.
Expert Tips
- Never squeeze: It ruptures follicles 10x more deeply, per dermatologists, guaranteeing scars—use hydrocolloid patches instead to draw out contents safely.
- Layer actives wisely: Alternate salicylic acid AM with benzoyl peroxide PM to unclog without irritation, building tolerance over 2 weeks.
- Prioritize barrier repair: Niacinamide serums reduce inflammation and PIH by 40-60% in studies, applied post-cleansing.
- Monitor hormones: If acne clusters pre-period or persists post-25, test for PCOS via bloodwork—spironolactone often resolves stubborn cases.
Conclusion
Understanding why pimples scar empowers proactive skincare, shifting from reactive popping to preventive healing that preserves smooth texture.
By addressing root causes like bacterial overgrowth and inflammation promptly, most long-term damage becomes avoidable, restoring confidence through consistent, evidence-based routines. Ultimately, while genetics set the stage, habits determine the outcome—gentle care and timely intervention turn potential scars into faint memories, proving acne need not define your skin's future.
Frequently Asked Questions
Can all pimples scar if left alone?
No, mild papules or pustules often heal without marks, but deep nodules/cysts scar in 20-50% of cases due to dermal rupture—treat aggressively early.
Does picking every pimple cause permanent damage?
Yes, mechanical trauma spreads bacteria and destroys collagen, converting 70% of superficial spots into atrophic scars; hands-off healing is key.
How long do post-acne marks last without treatment?
PIH fades in 3-6 months naturally, but scars persist indefinitely without lasers or peels—retinoids speed fading by promoting turnover.
Are hormonal pimples more likely to scar?
Absolutely; androgen-driven cysts rupture deeply, scarring 2-3x more than comedonal acne—anti-androgen treatments prevent this.