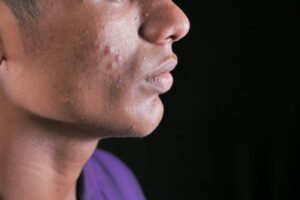
Acne treatments promise clearer skin, but for many, they deliver the opposite—more breakouts, redness, and frustration. This happens because common remedies like retinoids and benzoyl peroxide can irritate the skin, causing temporary flare-ups known as skin purging or irritation, while mismatched products or habits sabotage progress.
Understanding these pitfalls is crucial, as up to 50 million Americans battle acne annually, and improper treatment prolongs suffering and risks scarring. In this article, you will learn the top reasons your acne regimen might be backfiring, from incorrect diagnoses to lifestyle triggers, and how to spot skin purging versus true worsening. Armed with evidence-based insights, you will discover practical steps to fix your routine, expert tips for lasting results, and answers to common questions, empowering you to achieve clearer skin without the setbacks.
Table of Contents
- Why Is Your Acne Treatment Not Matching Your Skin's Needs?
- Could Skin Purging Be Fooling You Into Quitting Too Soon?
- Are Hidden Lifestyle Factors Undermining Your Routine?
- How Overdoing It Turns Treatments Against Your Skin
- The Role of External Triggers in Flare-Ups
- How to Apply This
- Expert Tips
- Conclusion
- Frequently Asked Questions
Why Is Your Acne Treatment Not Matching Your Skin's Needs?
Choosing the wrong treatment for your acne type or severity often leads to poor results or worsening breakouts. For instance, mild comedonal acne might respond to topicals alone, but severe cystic acne driven by hormones requires stronger interventions like isotretinoin, not just over-the-counter options. Mistaking acne for conditions like rosacea or fungal acne means applying irrelevant products that irritate pores further.
Treatments must align with your primary triggers—whether hormonal, bacterial, or inflammatory. Self-diagnosis frequently misses this, leading to mismatched regimens that fail to address root causes like excess sebum or clogged follicles. Initial irritation from actives like retinoids can mimic failure, but without proper adjustment, it escalates into chronic inflammation.
- Consult a dermatologist for accurate diagnosis, as stubborn acne may stem from PCOS, thyroid issues, or other imbalances misidentified as standard breakouts.
- Match severity: Topical benzoyl peroxide suits mild cases, while moderate-to-severe needs procedures like chemical peels or lasers.
- Test for acne variants: Hormonal acne demands anti-androgens or supplements, not just antibacterials.
Could Skin Purging Be Fooling You Into Quitting Too Soon?
Active ingredients like retinoids, salicylic acid, benzoyl peroxide, and vitamin C accelerate cell turnover, pushing trapped debris to the surface in a process called skin purging. This creates new breakouts that look worse initially, but it's a sign the treatment is working, typically lasting 4-6 weeks.
Overreacting by stopping leads to real regression, as the skin never reaches the clearing phase. Harsh overuse exacerbates this: too much benzoyl peroxide dries skin, prompting rebound oil production and clogged pores. Purging differs from irritation breakouts—pimples appear in usual zones, not randomly—and resolves with patience and buffering.
- Differentiate purging from allergies: Purging speeds up existing cycles; new rashes signal comedogenic ingredients like coconut oil.
- Buffer actives: Mix retinoids with moisturizer or apply every other night to minimize flare-ups.
Are Hidden Lifestyle Factors Undermining Your Routine?
Daily habits silently sabotage treatments by boosting oil, inflammation, and bacteria. Stress elevates cortisol, overstimulating sebaceous glands and creating a breakout cycle, especially when acne heightens self-consciousness.
Poor diet, like dairy or high-glycemic carbs, spikes IGF-1 and insulin, worsening sebum and pore-clogging. Comedogenic products in skincare, hair care, or makeup clog pores directly, while smoking impairs healing and alters the skin microbiome. Inconsistent application—skipping doses or spot-treating—halts progress, allowing acne to rebound.
- Cut dairy and refined sugars: Skim milk raises IGF-1; swap for plant alternatives to reduce inflammation.
- Manage stress: Prioritize sleep and relaxation to lower cortisol-driven oil surges.

How Overdoing It Turns Treatments Against Your Skin
Frequent changes or aggressive washing irritate the barrier, sparking rebound acne as skin compensates with excess oil. Picking pimples drives bacteria deeper, causing cysts and scars, while tight clothing or greasy environments trap oil.
Medications like corticosteroids or lithium indirectly fuel breakouts via hormonal shifts. Overloading with actives without moisturizing strips lipids, inviting inflammation—harsh scrubs worsen this vicious loop. Hormonal fluctuations from cycles, pregnancy, or PCOS amplify any regimen flaw, demanding tailored adjustments.
The Role of External Triggers in Flare-Ups
Environmental factors like high humidity or pollutants exacerbate oiliness, while hair products dripping onto the face block pores. Genetics play a part, making some prone to flare-ups from minor triggers, but lifestyle amplifies this.
Even "healthy" habits like frequent face-touching under stress transfer bacteria. Ignoring these turns treatments ineffective: a perfect topical routine fails amid poor hygiene or dietary sabotage.
How to Apply This
- Track your routine for two weeks: Note products, diet, stress, and breakouts to identify patterns like purging or triggers.
- Simplify and patch-test: Strip to basics—gentle cleanser, targeted active, moisturizer—introducing one change weekly.
- Seek professional input: Get a dermatologist diagnosis and customized plan, including hormone checks if flares are cyclic.
- Build consistency: Apply treatments fully to breakout zones nightly, buffer irritants, and log progress for 6-8 weeks minimum.
Expert Tips
- Moisturize religiously: Even oily skin needs non-comedogenic hydration to prevent rebound oil from drying treatments.
- Opt for non-comedogenic everything: Check labels for pore-clogging offenders like shea butter in lotions or conditioners.
- Incorporate anti-inflammatories: Add omega-3s from fish or flax to counter diet-driven flares.
- Time treatments wisely: Use actives at night; gentle antioxidants like vitamin C in mornings for barrier support.
Conclusion
Your acne treatment might worsen breakouts due to mismatches, purging, irritation from overuse, or overlooked triggers like diet and stress—but recognition is the first step to reversal. By aligning regimens with your skin's needs, building patience through purging phases, and addressing lifestyle saboteurs, clearer skin becomes achievable without endless trial-and-error.
Empower yourself with consistency and expert guidance to break the cycle. Sustainable skincare prioritizes barrier health and root causes, turning potential setbacks into pathways for lasting clarity.
Frequently Asked Questions
How long should I wait before deciding a treatment is failing?
Give it 6-8 weeks minimum; initial purging from retinoids or acids peaks at 4 weeks then improves—quitting early forfeits benefits.
Is dairy really causing my adult acne?
Studies link skim milk and dairy to IGF-1 spikes that boost sebum and inflammation, especially in hormonal acne—try eliminating for 4 weeks to test.
Can stress alone make acne treatments ineffective?
Stress raises cortisol, increasing oil and worsening existing acne, creating a loop that undermines topicals—pair routines with stress reduction for better results.
What's the difference between skin purging and a product allergy?
Purging brings faster breakouts in usual areas from cell turnover; allergies cause random redness, itching, or hives—discontinue irritants immediately.