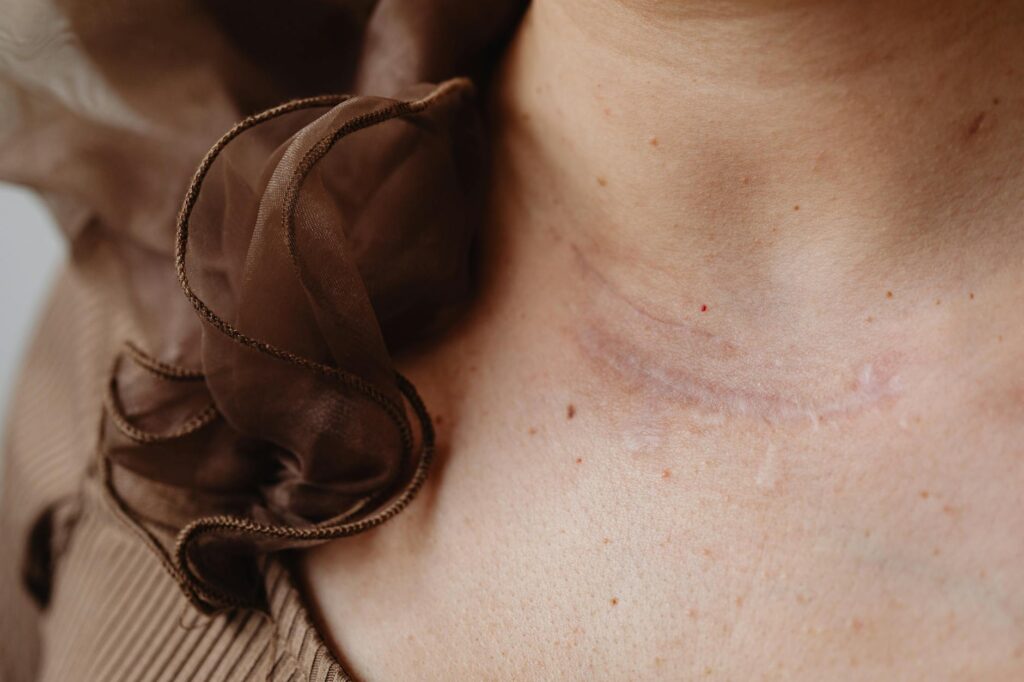
Complete acne scar removal is rarely possible because scars represent permanent structural damage to the dermis, the deep layer of skin that lacks the regenerative capacity to fully rebuild itself. When severe acne destroys collagen and tissue beneath the surface, the body patches the wound with fibrous scar tissue that differs fundamentally from the original skin architecture. Even the most advanced dermatological procedures, from fractional laser resurfacing to surgical subcision, typically achieve 50 to 70 percent improvement in scar appearance rather than total elimination. A person with deep ice pick scars across both cheeks, for instance, may see meaningful smoothing after a series of treatments, but close inspection will still reveal textural irregularities that betray the skin’s history.
This reality frustrates many people who spend thousands of dollars expecting flawless results, only to learn that “improvement” and “removal” are not the same thing. The skincare industry and even some clinics blur this distinction, advertising scar removal when they mean scar reduction. Understanding why the skin cannot fully regenerate after deep acne damage is essential for setting realistic expectations and making informed decisions about treatment. This article covers the biological reasons behind permanent scarring, how different scar types respond to treatment, what the most effective procedures can and cannot accomplish, and how to evaluate whether a treatment plan is worth pursuing.
Table of Contents
- Why Can’t the Skin Fully Repair Deep Acne Scars?
- How Scar Type Determines What Treatment Can Realistically Achieve
- What the Best Available Treatments Actually Deliver
- Evaluating Whether Scar Treatment Is Worth the Investment
- When Treatments Can Make Scars Worse Instead of Better
- The Role of Ongoing Skin Maintenance After Treatment
- What Emerging Research Suggests About the Future of Scar Treatment
- Conclusion
- Frequently Asked Questions
Why Can’t the Skin Fully Repair Deep Acne Scars?
The answer lies in a fundamental difference between how superficial wounds and deep wounds heal. When damage is confined to the epidermis, the outermost layer of skin, the body can regenerate tissue that is virtually identical to the original. A shallow scrape heals without a trace because epidermal cells divide rapidly and reconstruct themselves in organized layers. But when inflammation from cystic or nodular acne penetrates into the dermis or subcutaneous tissue, the destruction reaches structures the body cannot replicate, including the precise arrangement of collagen bundles, elastin fibers, blood vessels, and hair follicles that give skin its texture and resilience. Instead of true regeneration, the body defaults to a repair process that prioritizes speed over fidelity. Fibroblasts rush to the wound site and deposit collagen in a disorganized, parallel pattern rather than the basket-weave structure found in undamaged skin.
This produces scar tissue that is functionally adequate for sealing the wound but structurally inferior. In some cases, too little collagen is deposited, creating atrophic scars like rolling, boxcar, or ice pick types. In others, excess collagen forms raised hypertrophic or keloid scars. Neither outcome resembles the original skin. Compare this to a lizard regrowing its tail versus a human healing a deep cut. Humans simply do not possess the biological machinery to regenerate complex dermal architecture once it has been destroyed.
How Scar Type Determines What Treatment Can Realistically Achieve
Not all acne scars respond equally to treatment, and this is where expectations most often collide with reality. Rolling scars, which are broad depressions caused by fibrous bands tethering the skin to deeper tissue, tend to respond best to procedures like subcision and filler injections because the surrounding skin structure is relatively intact. Many patients with predominantly rolling scars see 60 to 75 percent improvement after a combination treatment series, and the results can be quite satisfying in real-world terms even if the skin is not perfectly smooth. Ice pick scars, by contrast, are narrow and deep, sometimes extending through the full thickness of the dermis.
These are among the most stubborn to treat because their geometry makes them resistant to resurfacing lasers, which work by vaporizing tissue layer by layer across a broad surface. A fractional CO2 laser session might soften the edges of an ice pick scar and reduce its depth by 20 to 30 percent, but it cannot fill a vertical channel of missing tissue. TCA cross, a technique where trichloroacetic acid is applied directly into the scar to stimulate collagen from the base up, tends to produce better results for ice pick scars, though it requires multiple sessions and improvement plateaus. However, if your scars are primarily shallow boxcar type, you are in a comparatively better position. These flat-bottomed depressions respond well to fractional lasers and punch excision, and some patients achieve results that are difficult to notice without close inspection in good lighting.
What the Best Available Treatments Actually Deliver
Fractional laser resurfacing, particularly ablative CO2 lasers like the Fraxel Repair and ActiveFX systems, remains the gold standard for broad acne scar improvement. Published clinical studies consistently show average improvement in the range of 40 to 70 percent after one to three sessions, measured by objective scar grading scales. A 2019 meta-analysis in the Journal of the American Academy of Dermatology reviewed 24 studies on fractional CO2 laser treatment for acne scars and found a pooled improvement rate of approximately 55 percent. That is a meaningful change, one that many patients describe as life-changing, but it is not erasure. Combination approaches tend to outperform any single treatment.
A dermatologist might perform subcision to release tethered scars, inject poly-L-lactic acid or hyaluronic acid filler to restore volume, apply TCA cross to individual ice pick scars, and follow up with a series of fractional laser sessions to improve overall texture. This layered strategy can push results toward the higher end of the improvement spectrum. One well-documented case at a university dermatology clinic involved a patient with severe mixed scarring who underwent subcision, filler, and three sessions of fractional CO2 laser over eighteen months. Independent reviewers graded the improvement at roughly 65 percent using the Goodman and Baron scar grading scale. The patient reported significantly improved confidence and quality of life, but the scars remained visible under direct overhead lighting.
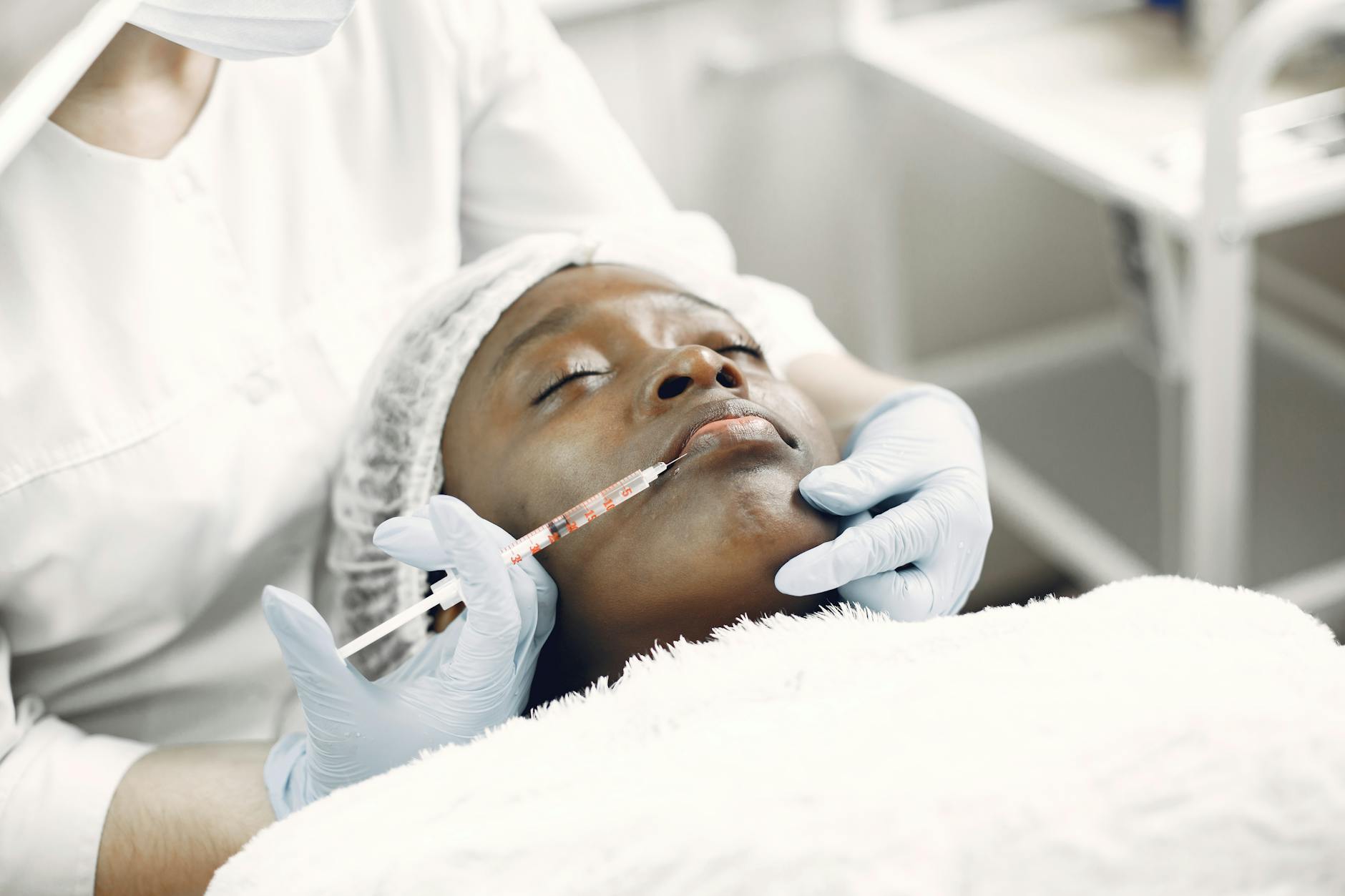
Evaluating Whether Scar Treatment Is Worth the Investment
The decision to pursue acne scar treatment involves balancing realistic improvement against cost, downtime, discomfort, and risk. A single fractional CO2 laser session typically costs between $1,000 and $3,000 depending on the treatment area and geographic location, and most patients need two to four sessions spaced six to eight weeks apart. Subcision runs $200 to $600 per session. Dermal fillers for volume loss range from $600 to $1,200 per syringe. A comprehensive combination plan for moderate to severe scarring can easily total $5,000 to $15,000 over the course of a year or more, and very little of this is covered by insurance. The tradeoff calculus differs dramatically based on scar severity.
Someone with mild, predominantly rolling scars might achieve results they are genuinely happy with after two or three laser sessions and a single round of subcision, spending perhaps $4,000 total. For that person, the investment may feel entirely worthwhile. But someone with severe, deep ice pick and boxcar scarring across the full face may spend $12,000 or more and still have visibly scarred skin, just less so. This is not a failure of the treatment but a reflection of biological limits. Before committing, ask your dermatologist to show you before-and-after photos of patients with similar scar types and severity, not the best-case portfolio shots on the clinic’s website. Also ask what percentage improvement they realistically expect for your specific case. Any provider who promises complete removal or uses the word “erase” should be approached with skepticism.
When Treatments Can Make Scars Worse Instead of Better
One underappreciated risk of aggressive scar treatment is the possibility of making things worse. Post-inflammatory hyperpigmentation is common after laser treatment, particularly in patients with darker skin tones, Fitzpatrick types IV through VI. In some cases, the pigmentation changes are more distressing than the original scars and can take months to resolve. More seriously, ablative lasers carry a small but real risk of causing new scarring if the treatment is too aggressive or the patient’s healing response is abnormal. Inexperienced providers sometimes apply the wrong treatment to the wrong scar type.
Dermabrasion or aggressive laser resurfacing on active cystic acne, for example, can spread infection and create fresh scars. Microneedling performed too deeply or with improper technique can cause track marks that look like tiny linear scars. Keloid-prone patients who undergo any procedure that creates new wounds risk developing hypertrophic or keloid scars that are more conspicuous than the acne scars they were trying to treat. This is why a thorough consultation that includes discussion of your skin type, healing history, and tendency toward abnormal scarring is not optional. If you have ever developed a keloid from a minor wound, ear piercing, or surgical incision, you need to communicate this explicitly and ensure your provider adjusts the treatment plan accordingly.

The Role of Ongoing Skin Maintenance After Treatment
Even after a successful treatment series, the appearance of acne scars is not static. Collagen remodeling continues for six to twelve months after the final laser or needling session, and consistent use of tretinoin (prescription retinoid) during this period has been shown to support continued improvement. A small controlled study found that patients who used tretinoin 0.05% nightly for six months post-laser showed approximately 10 to 15 percent additional improvement compared to those who used moisturizer alone.
Daily broad-spectrum sunscreen is equally critical during and after treatment. Ultraviolet exposure degrades collagen, accelerates skin aging, and worsens post-inflammatory pigmentation, all of which can undermine treatment gains. The irony is that many patients diligently follow their treatment schedule but neglect the daily maintenance that protects their investment. Think of it this way: scar treatment is an intervention, but the skin you live with long-term is shaped by what you do every day.
What Emerging Research Suggests About the Future of Scar Treatment
Researchers are exploring several promising avenues that could eventually push improvement rates beyond current limits. One area of active investigation involves the use of stem cell-derived growth factors applied topically after microneedling or laser treatment to enhance the quality of collagen produced during wound healing. Early-phase studies have shown encouraging results, though large-scale clinical trials are still needed. Another line of research focuses on the Engrailed-1 gene and the role of specific fibroblast subtypes in determining whether a wound heals with or without a scar.
Scientists at Stanford have demonstrated in animal models that inhibiting certain fibroblast signaling pathways can shift wound healing toward regeneration rather than scar formation. These developments are years or possibly decades away from clinical application, but they represent a genuine shift in how the field thinks about scarring. The current paradigm accepts scar tissue as an inevitable endpoint and focuses on remodeling it. The future paradigm may involve preventing scar formation entirely or converting existing scar tissue into normal skin at the cellular level. Until then, the honest answer remains that treatment can significantly improve acne scars but cannot make them disappear completely, and anyone who tells you otherwise is selling something.
Conclusion
Complete acne scar removal remains beyond the reach of current medicine because deep scarring involves permanent structural damage that the body patches rather than truly regenerates. The most effective treatment strategies, combining subcision, fillers, chemical reconstruction, and fractional laser resurfacing, can achieve meaningful improvement in the range of 50 to 70 percent for most patients. That improvement is real and often transformative for quality of life, but it is not the same as having skin that was never scarred. Understanding this distinction protects you from spending money chasing an impossible outcome and helps you appreciate the genuine progress that treatment can deliver.
If you are considering scar treatment, start with a consultation with a board-certified dermatologist who specializes in procedural dermatology or a fellowship-trained laser surgeon. Ask for honest assessments of expected improvement for your specific scar types, request to see before-and-after images of patients with comparable scarring, and discuss the full cost and timeline before committing. Prioritize providers who speak in terms of percentages and realistic outcomes rather than promises of flawless skin. And regardless of whether you pursue professional treatment, protect the skin you have now with daily sunscreen and a consistent retinoid, because preventing further damage is the one intervention that is both fully effective and entirely within your control.
Frequently Asked Questions
Can microneedling alone remove acne scars?
Microneedling can improve mild to moderate acne scars by stimulating collagen production, but it is generally less effective than fractional laser treatment for deeper scars. Studies show typical improvement of 30 to 50 percent after four to six sessions. It works best for shallow rolling scars and overall texture improvement, not for deep ice pick or boxcar scars.
How long does it take to see results from acne scar treatment?
Most treatments trigger a collagen remodeling process that continues for three to six months after each session. Visible improvement usually begins around the six-week mark, but final results from a full treatment series may not be apparent for twelve to eighteen months after the last procedure. Patience is genuinely required.
Are acne scar treatments safe for dark skin tones?
Many treatments carry higher risks of hyperpigmentation and hypopigmentation for patients with Fitzpatrick skin types IV through VI. Non-ablative fractional lasers, microneedling, and certain chemical peels tend to be safer options than ablative lasers for darker skin. An experienced provider who regularly treats diverse skin tones is essential for minimizing complications.
Do over-the-counter scar creams work on acne scars?
Most over-the-counter scar creams have little to no effect on true atrophic acne scars because these products cannot reach the deep dermal damage that causes the scarring. Silicone-based products may help flatten raised scars. Retinol serums can modestly improve skin texture over time, but they will not fill depressed scars. The claims on most drugstore scar products far exceed what the evidence supports.
Is it possible to get acne scar treatment while still having active breakouts?
It is generally not recommended. Active acne increases the risk of infection and new scarring from procedures. Most dermatologists want acne to be well controlled for at least three to six months before starting scar treatment. Treating active acne first also prevents new scars from forming while you are investing in treating existing ones.
At what age should someone start treating acne scars?
There is no strict age requirement, but most dermatologists recommend waiting until active acne has been controlled and the skin has had time to mature. For many people, this means starting scar treatment in the late teens to mid-twenties. Starting too early while acne is still active wastes money and risks creating additional damage.
You Might Also Like
- Why Tracking Acne Scar Progress at Home Requires Consistent Lighting
- Why Managing Expectations Is the Hardest Part of Acne Scar Treatment
- Why Acne Treatment Is Rarely Covered by Insurance — and How to Fight It
Browse more: Acne | Acne Scars | Adults | Back | Blackheads