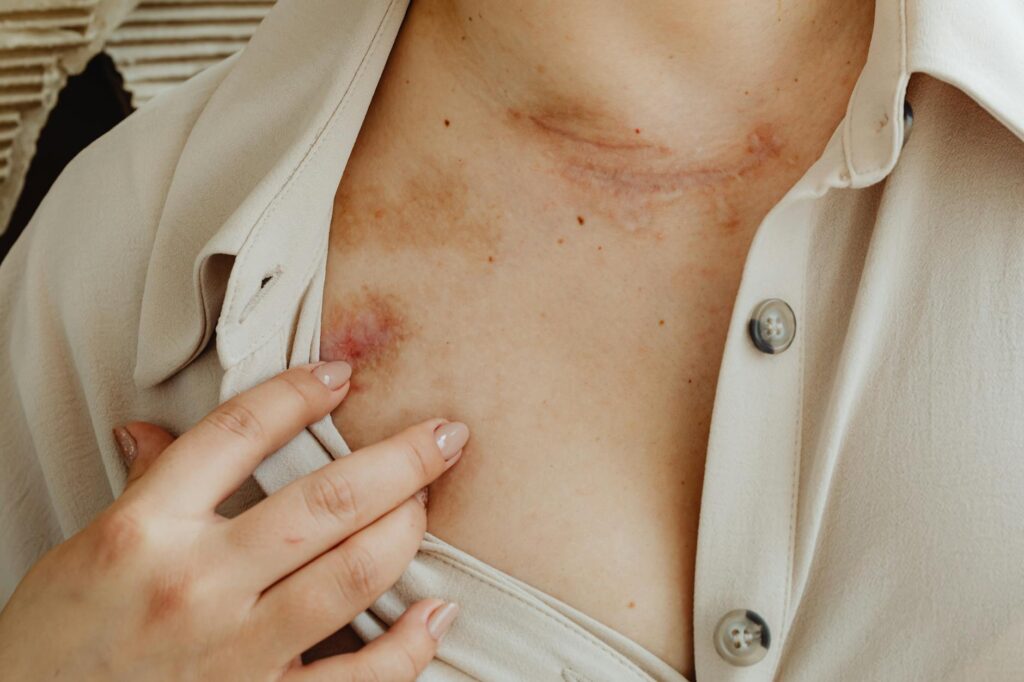
Aquaphor is recommended after laser scar treatment because it creates a breathable moisture barrier that prevents the irritation, infection, and dryness that would otherwise compromise your healing results. When your skin undergoes laser resurfacing for scars, the treatment creates controlled micro-injuries that trigger the body’s natural healing response. During this vulnerable window—typically the first two weeks—Aquaphor’s combination of petrolatum and panthenol keeps the treated area optimally hydrated while allowing new skin to grow underneath. This barrier function is why dermatologists consistently recommend it over alternatives like antibiotic ointments, which can actually interfere with the healing process.
The reason Aquaphor works better than many other post-treatment options comes down to a single, critical principle: moisture control. After laser treatment, your damaged skin is extremely susceptible to infection and excessive dryness, both of which can deepen scars or create new ones. Aquaphor’s lightweight, occlusive formula locks in the skin’s natural moisture without suffocating the area, which allows the new collagen and skin cells forming beneath the surface to develop uninterrupted. This article will walk you through exactly how Aquaphor works, when and how to apply it, the critical 2-week limit that many people overlook, and what comes after to maintain your scar-reduction progress.
Table of Contents
- How Does Aquaphor Create a Protective Barrier After Laser Scar Treatment?
- The Science Behind Aquaphor’s Healing Properties and Moisture Management
- Preventing Complications – Infection Risk and Optimal Wound Healing
- Applying Aquaphor Correctly – The Practical Timeline and Frequency Guide
- When Aquaphor Can Work Against You – Duration Limits and Pore Clogging Risks
- Transitioning Beyond Aquaphor – The Silicone Gel Phase for Long-Term Scar Remodeling
- What Not to Use – Common Mistakes That Delay Healing After Laser Treatment
- Conclusion
How Does Aquaphor Create a Protective Barrier After Laser Scar Treatment?
Aquaphor’s effectiveness lies in its specific formulation of petrolatum, which is a highly refined mineral oil, combined with panthenol, a form of vitamin B5 that actively soothes inflammation. Together, these ingredients form a breathable barrier—the key word being breathable, since your skin still needs oxygen to heal. Unlike plastic wrap or heavier ointments that trap sweat and bacteria, Aquaphor allows your skin to “breathe” while keeping moisture locked in at the cellular level. This balance is essential because after laser treatment, your skin’s natural protective barrier is temporarily compromised, making it vulnerable to irritants in the air, water, and bacteria that would normally be kept out. The petrolatum component is particularly important because it mimics the skin’s own lipid production. When laser treatment damages your skin, you lose some of this natural lipid layer, which is why the treated area feels so tight and uncomfortable.
By replenishing this layer with Aquaphor, you’re essentially giving your skin the raw materials it needs to rebuild itself. Panthenol adds another dimension by reducing inflammation and actually stimulating skin cell turnover, which is why it’s found in so many medical-grade post-procedure products. Think of it this way: if your scar-treated skin is a house with broken windows, Aquaphor is the plastic sheeting that keeps the weather out while the glazier comes to fix the windows. The breathability of Aquaphor also prevents the secondary damage that can occur when you use a truly occlusive product for too long. Some people, attempting to maximize hydration, use petroleum jelly or other heavier products for weeks after treatment. What actually happens is sweat and bacteria become trapped, creating the perfect environment for acne and folliculitis to develop—new scarring you didn’t have before. Aquaphor’s formulation avoids this by having a slightly lighter texture that allows moisture to evaporate while still maintaining that critical protective layer.

The Science Behind Aquaphor’s Healing Properties and Moisture Management
Your skin after laser treatment is in a heightened state of water loss, a process called transepidermal water loss (TEWL). The laser has disrupted the outermost layers where moisture is normally retained, so water is literally evaporating from your skin faster than at any other time in your life. Aquaphor works by slowing this water loss to near-normal levels, which keeps the healing environment stable. This is why moisture-barrier products are considered medically essential post-laser, not optional—without them, the wound becomes overly dry, which can cause the tissue to scar more heavily and can even cause the healing to go backward, creating increased redness and texture. However, if you’re prone to very oily skin or have a history of clogged pores, know that even Aquaphor can cause some congestion if overused. This is where duration becomes critical—which we’ll cover in detail later.
The science supports using Aquaphor for the first two weeks when infection risk is highest and the wound is most fragile, but past that point, the risk-benefit ratio flips. Your skin is no longer a raw wound; it’s transitioning into the remodeling phase where silicone-based products become more appropriate. Trying to keep the area locked in Aquaphor’s occlusive environment for months is counterproductive and can actually slow the final maturation of the scar tissue. One often-overlooked aspect of moisture management is that it needs to be done correctly to matter at all. If you apply Aquaphor to completely dry skin in a rushed manner, you’re just smearing it on top rather than integrating it into the skin barrier. The recommended practice is to apply Aquaphor to skin that’s slightly damp from cleansing, which allows it to absorb more effectively and distribute more evenly. This makes a measurable difference in how well the barrier works.
Preventing Complications – Infection Risk and Optimal Wound Healing
Infection is one of the most serious post-laser complications because it can cause permanent scarring, discoloration, and even spread deeper into the skin. Keeping the wound continuously moist with Aquaphor is one of the primary strategies dermatologists use to prevent infection. This might seem counterintuitive—doesn’t moisture encourage bacteria?—but the answer is nuanced. What encourages bacterial growth is stagnant moisture trapped under a completely occlusive layer. What Aquaphor does is maintain a clean, moist environment that promotes your skin’s own healing cells to work faster than any bacteria can establish a foothold. Your newly forming skin cells create antimicrobial compounds and are constantly repairing the barrier, which is faster than typical bacteria can overtake. Beyond infection prevention, continuous moisture also ensures that new skin cells—called keratinocytes—can migrate across the healing wound more smoothly.
These cells are responsible for generating collagen and elastin, which are what actually repair scar tissue. In a dry environment, these cells move slowly and inefficiently, causing unorganized collagen deposition, which deepens the scar. In an optimally moist environment maintained by Aquaphor, they work at peak efficiency. Studies on wound healing consistently show that moist wound management produces better outcomes than allowing wounds to “air out,” which is why Aquaphor’s approach is considered the gold standard. That said, if you notice any signs of actual infection—pus, spreading redness, warmth, or systemic symptoms like fever—Aquaphor cannot replace medical attention. Stop use immediately and contact your dermatologist. Aquaphor’s moisture barrier prevents the vast majority of infections from occurring in the first place, but it is not an antibiotic and cannot treat an existing infection. This is also why people are specifically advised against using topical antibiotics like Neosporin: they can mask early signs of infection and also potentially delay the skin’s own healing response.
Applying Aquaphor Correctly – The Practical Timeline and Frequency Guide
The clinical recommendation is to begin Aquaphor application immediately after your laser treatment—ideally within the first hour—and continue continuously for the first 24 hours. This means reapplying every few hours, not just once before bed. Many dermatology clinics specifically instruct patients to apply it continuously during this critical initial window because the wound is at its most vulnerable point. If you’re treating scars at home with at-home laser devices, follow the same timeline: treat and then immediately apply Aquaphor. After that initial 24-hour period, the frequency drops to 2-3 times daily, with the most important applications being immediately after cleansing and before bed. This is because cleansing removes the previous layer of Aquaphor along with dead skin and bacteria, so reapplication right after is essential for maintaining that barrier.
The pre-bed application ensures your skin goes into its naturally most-active repair phase (circadian rhythm increases cellular turnover at night) with optimal moisture protection. Additionally, if you notice the treated area starting to feel tight or uncomfortably dry between regular applications, you should reapply immediately—your skin is telling you the barrier needs reinforcement. A practical tip that many people miss: use clean fingertips or a clean applicator when applying Aquaphor, not your whole hand. This reduces the chance of introducing bacteria into the wound. Some dermatologists recommend a very thin layer rather than a thick one, because the goal is barrier protection, not occlusion. A thick layer actually sits on top of the skin rather than forming an integrated barrier, and it’s more likely to pick up bacteria and dirt. Think of it as creating a light seal rather than plastering the area.
When Aquaphor Can Work Against You – Duration Limits and Pore Clogging Risks
Here’s the critical fact that separates proper post-laser care from amateur wound care: do not use Aquaphor for more than 2 weeks after treatment. This is not a suggestion or a guideline with wiggle room—it’s a clinical boundary based on the changing needs of your healing skin. After 14 days, the wound has transitioned from an acute injury phase to a remodeling phase. Your skin is no longer fragile; new blood vessel networks have formed, the surface has begun to re-epithelialize, and infection risk has dropped dramatically. Continuing with Aquaphor’s heavy occlusion past this point actively works against you because it can clog pores, trap bacteria, and potentially cause acne—creating new scarring that competes with the existing scar you were trying to treat. The pore-clogging issue is particularly relevant if you have oily or acne-prone skin. After 2 weeks, your skin cells are more resilient and your glands are starting to function normally again.
If Aquaphor is still sealing everything off, sebum and dead skin cells get trapped inside pores, creating comedones. In some cases, this leads to inflammatory acne that leaves its own scars. It’s a perverse outcome: you followed the post-laser instructions perfectly, but by being overly diligent, you created a new problem. This is why the transition at the 2-week mark is crucial. What should you switch to instead? Silicone gel therapy becomes the next phase of scar management. Silicone-based products (such as silicone gel sheets or topical silicone serums) continue to support scar remodeling but without the pore-clogging risk that comes with petrolatum. They work through a completely different mechanism—hydration and collagen organization rather than barrier occlusion. Make a note of your treatment date and set a calendar reminder for 2 weeks out to switch products, so you don’t accidentally extend Aquaphor use past its usefulness window.

Transitioning Beyond Aquaphor – The Silicone Gel Phase for Long-Term Scar Remodeling
The transition from Aquaphor to silicone therapy marks a shift in your scar’s healing timeline. In the first two weeks, you’re prioritizing acute wound protection and infection prevention. From week 3 onward, your focus moves to scar remodeling—the process of reorganizing collagen, flattening texture, and improving appearance. Silicone-based products work differently than Aquaphor; they hydrate the scar tissue directly, which causes collagen fibers to relax and reorganize into a more normal pattern. They’re also non-occlusive, so they won’t clog pores or trap moisture in the way Aquaphor would if used long-term. Silicone gels come in two main forms: sheets (which you apply to the scar for 12+ hours daily) and topical serums (which you apply like a moisturizer).
Both are scientifically supported for scar improvement and are often used for months or even longer if needed. The advantage of switching at the 2-week mark is that you’re applying them to skin that’s already substantially healed from the acute trauma but is still in the active remodeling window, when interventions tend to be most effective. If you wait months to start silicone therapy, the scar has already begun to harden and become more resistant to flattening. Some dermatologists recommend starting silicone therapy overlapping slightly with the end of Aquaphor use—for example, applying silicone serum on day 10-12 while still using Aquaphor, then discontinuing Aquaphor at day 14. This gives your skin a gradual transition and ensures no gap in scar management. Check with your specific dermatologist on timing, as it can vary based on the laser used and your skin’s specific response.
What Not to Use – Common Mistakes That Delay Healing After Laser Treatment
Almost as important as knowing what to use is knowing what to avoid. Hydrogen peroxide and alcohol-based products should never be applied to laser-treated skin during the healing phase, despite their reputation as “wound cleaners.” Both are extremely drying and irritating to compromised skin. Hydrogen peroxide, in particular, actually slows healing by creating free radicals that damage new skin cells faster than they can be replaced. If you need to cleanse the area, use only gentle, lukewarm water or a mild, fragrance-free cleanser—nothing more. Save the disinfectants for before the treatment, not after. Another common mistake is using Neosporin or other over-the-counter antibiotic ointments instead of Aquaphor. Many people assume that antibiotic coverage is protective after laser treatment, but dermatologists typically advise against this.
The antibiotic ingredients in Neosporin can trigger allergic reactions or contact dermatitis in already-sensitive post-laser skin, and there’s emerging evidence that topical antibiotics may interfere with the skin’s own immune response to minor contamination. If your dermatologist specifically prescribes an antibiotic ointment for you—which is different from general use—follow that guidance. But for routine post-laser care without any sign of infection, Aquaphor is the evidence-based choice. A third mistake is attempting “scar remedies” from internet recommendations during this acute phase. This is not the time to use vitamin C serums, retinoids, chemical exfoliants, or essential oils. Many of these products are irritating on normal skin and can cause severe reactions on freshly laser-treated skin. The most common result is inflammation that actually deepens the scar. Your only focus for the first 2 weeks should be healing and barrier protection—everything else comes later.
Conclusion
Aquaphor is recommended after laser scar treatment because it delivers the exact three things your healing skin needs: moisture retention, infection prevention, and a breathable protective barrier—all without the irritation or pore-clogging risk of heavier alternatives. Its specific formulation of petrolatum and panthenol has made it the gold standard in dermatology for post-laser wound management. By applying it 2-3 times daily for the first 2 weeks following treatment, you’re giving your skin the optimal environment for collagen repair and new cell growth, which directly translates to less visible scarring and faster recovery.
The key to success is respecting the 2-week boundary and transitioning to silicone-based scar therapy afterward, while avoiding common pitfalls like hydrogen peroxide, extended Aquaphor use, and internet remedies. Your laser treatment has already done the hard work of triggering healing; Aquaphor’s job is to protect that process and allow it to complete efficiently. With proper post-care, most laser treatments show their best results 3-6 months out, when the skin has fully remodeled and collagen has settled into its new, more organized structure.
You Might Also Like
- What Combination Scar Treatment Protocols Look Like
- Why Under-Eye Hollowing Worsens After Laser for Acne Scars
- What to Put on Your Face After CO2 Laser for Scars
Browse more: Acne | Acne Scars | Adults | Back | Blackheads