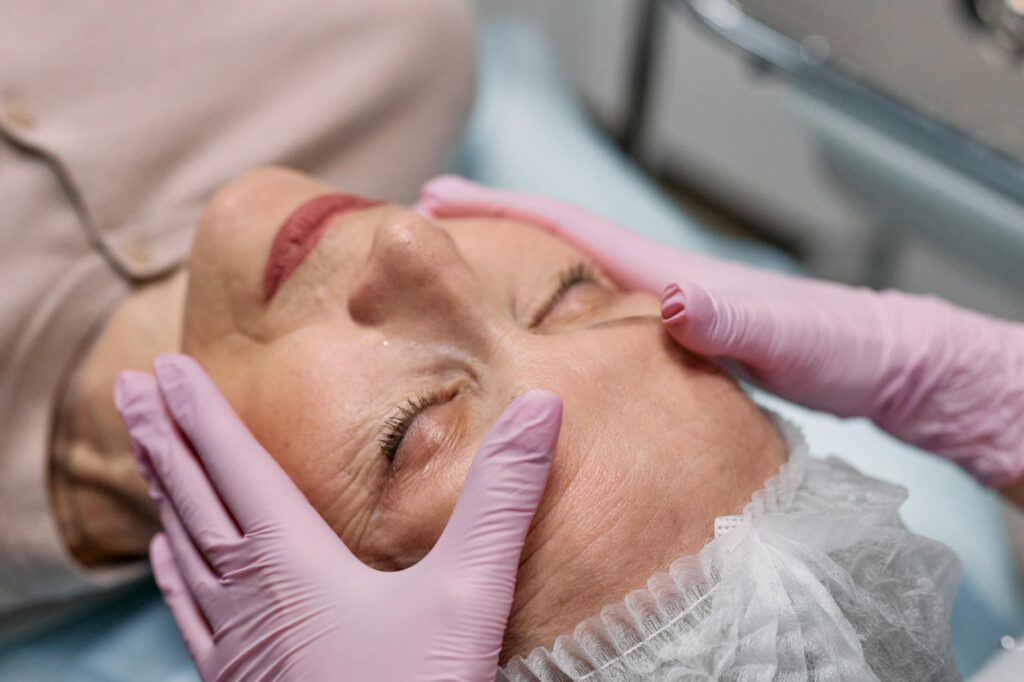
Using strong acne treatments and skincare products too often causes the opposite of what you want—damaged skin, resistant bacteria, and painful dependency cycles. Overuse doesn’t lead to better results faster; it triggers side effects like skin thinning, rashes that rebound worse when you stop, dangerous bacterial resistance, and compromised skin barriers that leave you more vulnerable to irritation and infection. Your skin’s healing comes from consistent, measured use of targeted treatments, not aggressive daily bombardment. This article covers what physically happens to your skin when you push treatments beyond safe limits, how overuse creates drug resistance and dependency, and why timing and frequency matter more than strength alone.
Table of Contents
- How Antibiotic Overuse Damages Your Skin and Gut
- Steroid Dependency and the Rebound Effect
- Breaking Your Skin Barrier with Aggressive Exfoliation
- When Frequency Becomes Harmful—Signs You’re Overdoing It
- Medication Overuse Headaches and Systemic Side Effects
- The Risk-Benefit Calculation for Strong Treatments
- Building a Sustainable Skincare Routine After Overuse
- Conclusion
How Antibiotic Overuse Damages Your Skin and Gut
Overusing prescription antibiotics for acne—especially oral antibiotics like doxycycline and minocycline—rewires your body’s defenses in dangerous ways. The bacteria you’re trying to kill adapt and become resistant to the medication, meaning the antibiotic stops working for you and anyone else who receives it. Even worse, antibiotics don’t discriminate; they kill beneficial bacteria in your gut alongside acne-causing bacteria, leading to yeast infections, digestive problems, and in severe cases, dangerous infections like *Clostridioides difficile* (C. difficile) colitis.
Unnecessary antibiotic use also increases your risk of serious infections that are harder to treat because resistant bacteria are now present in your body. The resistance problem extends beyond you. When you overuse antibiotics, you contribute to a global public health crisis; bacteria that evolve resistance in your body can spread to others. Dermatologists now recommend limiting oral antibiotics to 3–6 months maximum and using them only with benzoyl peroxide or retinoids, which make resistance less likely. If your dermatologist prescribed antibiotics for months or years, that’s overuse, and it’s worth a conversation about stepping down to topical treatments instead.

Steroid Dependency and the Rebound Effect
Topical corticosteroids are powerful anti-inflammatory treatments, but using them too frequently or on large areas of skin creates steroid dependency—a vicious cycle where your skin improves while you’re using the steroid, but worsens significantly when you stop. This happens because the steroid suppresses your skin’s natural inflammatory response, and when you discontinue it, inflammation returns stronger than before, often worse than the original condition. Prolonged overuse of high-potency corticosteroids causes permanent skin changes: thinning of the epidermis, visible stretch marks, easy bruising, wrinkling, and acne-like bumps that didn’t exist before treatment.
Long-term overuse also triggers secondary skin conditions, including rosacea, perioral dermatitis (a painful rash around the mouth), and purpura (dark purple spots from fragile blood vessels). The skin can also develop a burning sensation and worsening of certain infections, particularly fungal infections that thrive in damaged barrier skin. If you’ve been using a potent corticosteroid cream daily for weeks or months, your skin has likely become dependent, and abruptly stopping will cause a flare that can last longer than your original problem. Stepping down requires a slow taper under dermatology guidance, not cold turkey.
Breaking Your Skin Barrier with Aggressive Exfoliation
Exfoliating treatments—including chemical exfoliants like AHAs and BHAs, vitamin C serums, and physical scrubs—serve a purpose when used appropriately. However, overuse destroys your skin’s protective barrier, the outermost layer of lipids and dead skin cells that keep irritants out and moisture in. Once this barrier is compromised, you’re left with increased sensitivity, inflammation, dermatitis, and a face that reacts angrily to everything else you apply. A compromised barrier also allows bacterial overgrowth because the skin can’t defend itself naturally.
The warning here is that aggressive exfoliation feels productive—your skin looks bright and smooth immediately after—but this false confidence leads to daily or twice-daily use. Within weeks, your skin is raw, sensitive, and burning. Recovery requires stopping exfoliation entirely and focusing on barrier repair with gentle cleansing, moisturizers, and sometimes prescription barrier repair creams. The irony is that you end up irritated and unable to use acne treatments at all while you heal.
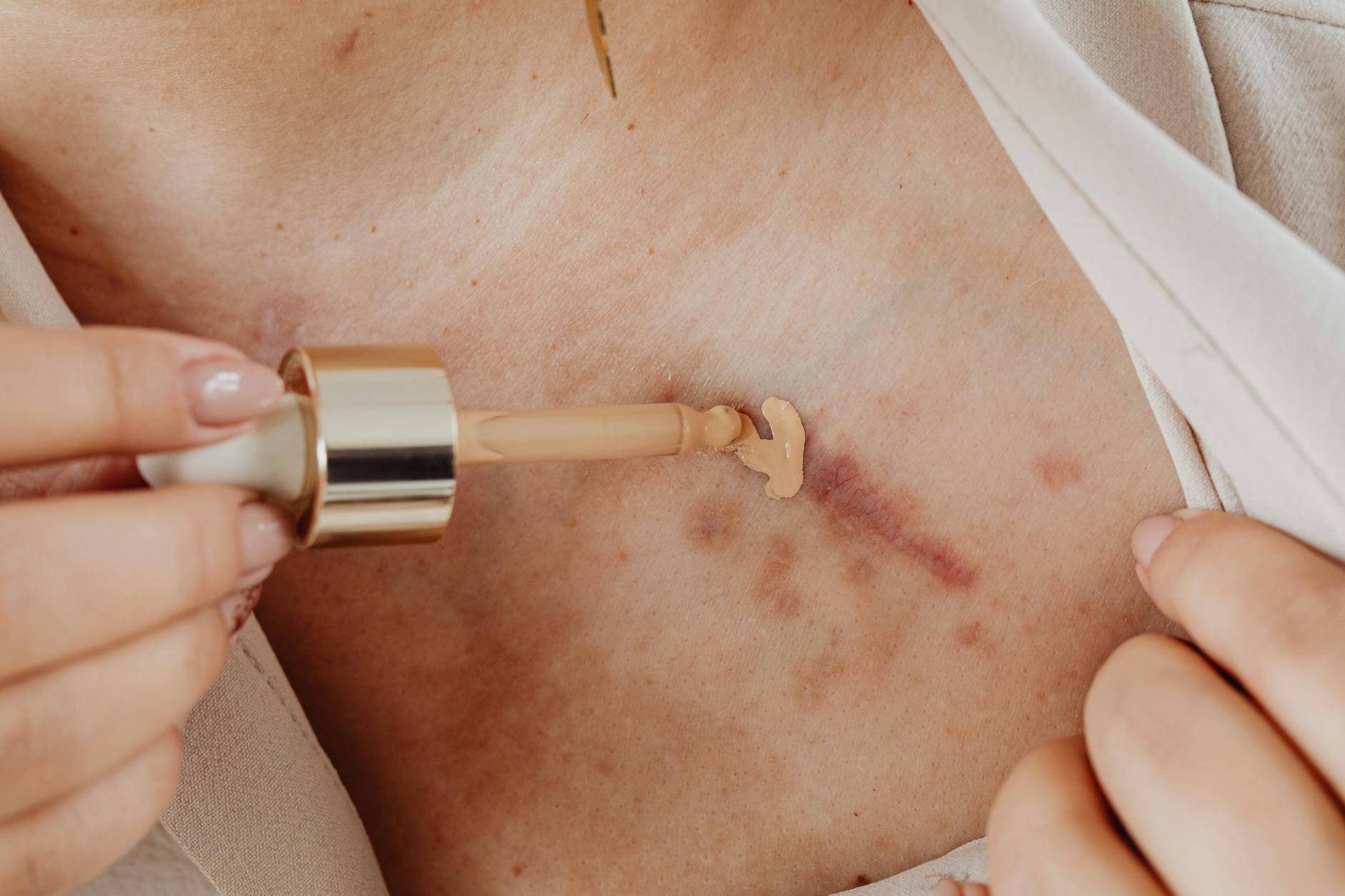
When Frequency Becomes Harmful—Signs You’re Overdoing It
Your treatment is likely overused if you experience any of these: increased dryness, flaking, or peeling; burning or stinging that doesn’t improve within the first week; new acne-like bumps or rashes; persistent redness or flushing; or mood changes in skin that cycle between clear and severely inflamed. Overuse also manifests as thinning skin that appears fragile, visible blood vessels, or increased sensitivity to sun and common skincare ingredients. Many people mistake these signs for the treatment “working” and increase the dose further, deepening the damage.
The comparison is straightforward: one application of a strong retinoid per week can clear acne over months without side effects; three applications per day causes barrier damage, flaking, and inflammation that prevents healing. More frequent use doesn’t accelerate results—it triggers protective inflammation that makes acne worse. Dermatologists recommend starting low and slow: once or twice weekly for strong actives, increasing frequency only if your skin tolerates it after 4–6 weeks. If you’re not seeing improvement at conservative doses, the problem usually isn’t frequency; it’s the wrong active ingredient for your skin type.
Medication Overuse Headaches and Systemic Side Effects
Beyond topical treatments, overusing oral medications—particularly over-the-counter pain relievers taken daily or near-daily—causes medication overuse headaches, a rebound headache disorder where the medication itself triggers the pain it’s meant to treat. This cycle compounds when the pain reliever is used for stress-related or hormonal acne; you’re taking it daily, your body becomes dependent, and withdrawal causes worse pain and flare-ups. Side effects from chronic medication use also include drowsiness that impairs your ability to drive and work, which creates a functional problem beyond skin health.
Research shows that nearly 50% of primary care physicians report their patients receive excessive medical care, often including unnecessary or overused medications. If you’re using acne medication daily for years, it’s worth asking your dermatologist whether stepping down to targeted, shorter-term use is possible. Some treatments are designed for short-term use (like antibiotics); others are maintenance treatments (like retinoids), but even retinoids can be reduced to lower frequencies once skin improves. The goal is using the lowest effective dose, not the most aggressive regimen.

The Risk-Benefit Calculation for Strong Treatments
Strong treatments exist because sometimes acne severity justifies their risks—severe cystic acne or widespread inflammatory acne may require Accutane, high-dose antibiotics, or powerful topical steroids. The risk-benefit calculation shifts when acne is mild to moderate or when overuse is happening without corresponding improvement. If you’ve been using the same strong treatment for years without acne improving, the treatment isn’t working, and continuing is pure risk.
This is where working with a dermatologist matters. They can evaluate whether your current regimen is actually addressing the acne or just causing damage. Sometimes switching to a different mechanism (like trying benzoyl peroxide instead of more antibiotics) solves the problem without the downsides of overuse. The limitation is that some people delay seeing a dermatologist and self-treat for years, assuming that more aggressive measures will eventually work.
Building a Sustainable Skincare Routine After Overuse
If you’ve damaged your skin through overuse, recovery is slow but possible. The first step is stopping the offending treatment entirely and allowing your barrier and skin microbiome to regenerate—this takes 2–4 weeks minimum. During this time, use only gentle cleansing and basic moisturizing; resist the urge to introduce new treatments. Once your skin stabilizes, reintroduce treatments one at a time, at low frequencies, and with patience.
A sustainable routine for acne-prone skin uses one active treatment (retinoid, AHA/BHA, or benzoyl peroxide) at appropriate frequency, not multiple actives daily. The forward-looking insight is that acne treatment is a marathon, not a sprint. The most successful long-term outcomes come from consistency at moderate doses over months, not aggressive short-term blitzes. Your skin heals and adapts better to treatments you use 2–3 times weekly than to daily high-potency applications. Building this mindset—prioritizing skin health alongside acne control—prevents the overuse cycle from repeating.
Conclusion
Using strong treatments too often causes skin damage, bacterial resistance, treatment dependency, and paradoxically, worse acne. The specific harms vary—antibiotics create resistance and gut problems; steroids cause thinning, dependency, and secondary skin conditions; exfoliants destroy your barrier—but the pattern is consistent: overuse triggers side effects that prevent the treatment from working. The answer to “how do I clear my acne faster” is rarely “more aggressive treatment”; it’s usually “the right treatment at the right frequency.” If you’re experiencing side effects from your current routine, the first step is honest evaluation with a dermatologist.
Together, you can identify which treatments are worth the risk and which are causing more harm than benefit. Clearing acne while protecting your skin’s health is possible, but it requires restraint and evidence-based dosing, not intensity. Start low, go slow, and give treatments time to work—your skin will thank you with clearer, healthier results.
You Might Also Like
- What Happens When You Combine Too Many Treatments for Redness
- Why Laser Treatments Are Used for Persistent Redness
- What Happens When You Treat Redness With Harsh Ingredients
Browse more: Acne | Acne Scars | Adults | Back | Blackheads